
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Complications
- The Risk of Diabetes on Clinical Outcomes in Patients with Coronavirus Disease 2019: A Retrospective Cohort Study
- Seung Min Chung, Yin Young Lee, Eunyeong Ha, Ji Sung Yoon, Kyu Chang Won, Hyoung Woo Lee, Jian Hur, Kyung Soo Hong, Jong Geol Jang, Hyun Jung Jin, Eun Young Choi, Kyeong-Cheol Shin, Jin Hong Chung, Kwan Ho Lee, June Hong Ahn, Jun Sung Moon
- Diabetes Metab J. 2020;44(3):405-413. Published online May 21, 2020
- DOI: https://doi.org/10.4093/dmj.2020.0105
- 10,201 View
- 143 Download
- 43 Web of Science
- 45 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background To determine the role of diabetes mellitus (DM) in the coronavirus disease 2019 (COVID-19), we explored the clinical characteristics of patients with DM and compared risk factors such as age, glycemic control, and medications to those without DM.
Methods This was a retrospective cohort study of 117 confirmed patients with COVID-19 which conducted at a tertiary hospital in Daegu, South Korea. The primary outcome was defined as the severe and critical outcome (SCO), of which the composite outcomes of acute respiratory distress syndrome, septic shock, intensive care unit care, and 28-day mortality. We analyzed what clinical features and glycemic control-related factors affect the prognosis of COVID-19 in the DM group.
Results After exclusion, 110 participants were finally included. DM patients (
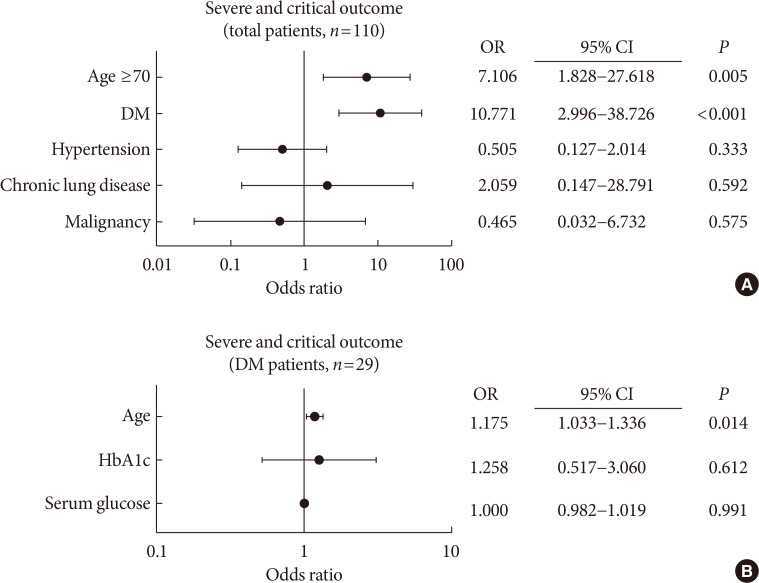
n =29) was older, and showed higher blood pressure compared to non-DM patients. DM group showed higher levels of inflammation-related biomarkers and severity score, and highly progressed to SCO. After adjustment with other risk factors, DM increased the risk of SCO (odds ratio [OR], 10.771;P <0.001). Among the DM patients, SCO was more prevalent in elderly patients of ≥70 years old and age was an independent risk factor for SCO in patients with DM (OR, 1.175;P =0.014), while glycemic control was not. The use of medication did not affect the SCO, but the renin-angiotensin system inhibitors showed protective effects against acute cardiac injury (OR, 0.048;P =0.045).Conclusion The COVID-19 patients with DM had higher severity and resulted in SCO. Intensive and aggressive monitoring of COVID-19 clinical outcomes in DM group, especially in elderly patients is warranted.
-
Citations
Citations to this article as recorded by- Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
Hyeyeon Moon, Sunghwan Suh, Mi Kyoung Park
Journal of Korean Medical Science.2023;[Epub] CrossRef - Severity of Symptoms and Mortality in Diabetic Patients with COVID- 19 Infection. Review
Zahraa ALBasry, Abeer Abdulhadi Rashid, Shaymaa Hasan Abbas
Al Mustansiriyah Journal of Pharmaceutical Sciences.2023; 23(1): 91. CrossRef - Risk phenotypes of diabetes and association with COVID-19 severity and death: an update of a living systematic review and meta-analysis
Sabrina Schlesinger, Alexander Lang, Nikoletta Christodoulou, Philipp Linnerz, Kalliopi Pafili, Oliver Kuss, Christian Herder, Manuela Neuenschwander, Janett Barbaresko, Michael Roden
Diabetologia.2023; 66(8): 1395. CrossRef - COVID-19 and Cardiovascular Comorbidities
Dirk Müller-Wieland, Nikolaus Marx, Michael Dreher, Katharina Fritzen, Oliver Schnell
Experimental and Clinical Endocrinology & Diabetes.2022; 130(03): 178. CrossRef - Prevalence and impact of diabetes in hospitalized COVID‐19 patients: A systematic review and meta‐analysis
Sian A. Bradley, Maciej Banach, Negman Alvarado, Ivica Smokovski, Sonu M. M. Bhaskar
Journal of Diabetes.2022; 14(2): 144. CrossRef - Does metformin affect outcomes in COVID‐19 patients with new or pre‐existing diabetes mellitus? A systematic review and meta‐analysis
Adithan Ganesh, Michael D. Randall
British Journal of Clinical Pharmacology.2022; 88(6): 2642. CrossRef - Cardioprotective effect of extracellular vesicles derived from ticagrelor-pretreated cardiomyocyte on hyperglycemic cardiomyocytes through alleviation of oxidative and endoplasmic reticulum stress
Ceylan Verda Bitirim, Zeynep Busra Ozer, Dunya Aydos, Kardelen Genc, Seyma Demirsoy, Kamil Can Akcali, Belma Turan
Scientific Reports.2022;[Epub] CrossRef - Impact of diabetes on COVID‐19 mortality and hospital outcomes from a global perspective: An umbrella systematic review and meta‐analysis
Stavroula Kastora, Manisha Patel, Ben Carter, Mirela Delibegovic, Phyo Kyaw Myint
Endocrinology, Diabetes & Metabolism.2022;[Epub] CrossRef - Glycated Albumin and Glycated Albumin/HbA1c Predict the Progression of Coronavirus Disease 2019 from Mild to Severe Disease in Korean Patients with Type 2 Diabetes
Jeongseon Yoo, Youngah Choi, Shin Ae Park, Ji Yeon Seo, Chul Woo Ahn, Jaehyun Han
Journal of Clinical Medicine.2022; 11(9): 2327. CrossRef - Novel Glycemic Index Based on Continuous Glucose Monitoring to Predict Poor Clinical Outcomes in Critically Ill Patients: A Pilot Study
Eun Yeong Ha, Seung Min Chung, Il Rae Park, Yin Young Lee, Eun Young Choi, Jun Sung Moon
Frontiers in Endocrinology.2022;[Epub] CrossRef - Renin‐Angiotensin Aldosterone System Inhibitors and COVID‐19: A Systematic Review and Meta‐Analysis Revealing Critical Bias Across a Body of Observational Research
Jordan Loader, Frances C. Taylor, Erik Lampa, Johan Sundström
Journal of the American Heart Association.2022;[Epub] CrossRef - The relationship of age, sex and prothrombin time related to the severity and mortality of COVID-19 patients with diabetes mellitus: a systematic review and meta analysis
Audrey Fabianisa Mirza, Ceria Halim, Mutiara Indah Sari
F1000Research.2022; 11: 729. CrossRef - Evaluating the effect of COVID-19 on quality measures of patients with type 2 diabetes in two family nurse practitioner–owned clinics
Wendy L. Wright, Patricia A. White, Meredith Welsh, Kelly Cutting
Journal of the American Association of Nurse Practitioners.2022; 34(9): 1090. CrossRef - Early glycaemic variability increases 28-day mortality and prolongs intensive care unit stay in critically ill patients with pneumonia
Seong Ho Kim, Ji Young Kim, Eun Song Kim, Il Rae Park, Eun Yeong Ha, Seung Min Chung, Jun Sung Moon, Ji Sung Yoon, Kyu Chang Won, Hyoung Woo Lee
Annals of Medicine.2022; 54(1): 2724. CrossRef - Anti-inflammatory drugs and the renin-angiotensin-aldosterone system: Current knowledge and potential effects on early SARS-CoV-2 infection
Iris Louise N. Cabbab, Rafael Vincent M. Manalo
Virus Research.2021; 291: 198190. CrossRef - The Effect of Prior Angiotensin-Converting Enzyme Inhibitor and Angiotensin Receptor Blocker Treatment on Coronavirus Disease 2019 (COVID-19) Susceptibility and Outcome: A Systematic Review and Meta-analysis
Jiuyang Xu, Yaqun Teng, Lianhan Shang, Xiaoying Gu, Guohui Fan, Yijun Chen, Ran Tian, Shuyang Zhang, Bin Cao
Clinical Infectious Diseases.2021; 72(11): e901. CrossRef - Diabetes predicts severity of COVID‐19 infection in a retrospective cohort: A mediatory role of the inflammatory biomarker C‐reactive protein
Huilin Koh, Angela Mei Chung Moh, Ester Yeoh, Yi Lin, Serena Kiat Mun Low, Say Tat Ooi, Seng Kiong Tan, Jaime Hui Xian Lin, Caroline Wei Shan Hoong
Journal of Medical Virology.2021; 93(5): 3023. CrossRef - Susceptibility for Some Infectious Diseases in Patients With Diabetes: The Key Role of Glycemia
Jesús Chávez-Reyes, Carlos E. Escárcega-González, Erika Chavira-Suárez, Angel León-Buitimea, Priscila Vázquez-León, José R. Morones-Ramírez, Carlos M. Villalón, Andrés Quintanar-Stephano, Bruno A. Marichal-Cancino
Frontiers in Public Health.2021;[Epub] CrossRef - Diabetes is most important cause for mortality in COVID-19 hospitalized patients: Systematic review and meta-analysis
Giovanni Corona, Alessandro Pizzocaro, Walter Vena, Giulia Rastrelli, Federico Semeraro, Andrea M Isidori, Rosario Pivonello, Andrea Salonia, Alessandra Sforza, Mario Maggi
Reviews in Endocrine and Metabolic Disorders.2021; 22(2): 275. CrossRef - COVID-19 and diabetes: Analysis of the scientific production indexed in Scopus
Ibraín Enrique Corrales-Reyes, Frank Hernández-García, Christian R. Mejia
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2021; 15(3): 765. CrossRef - Impact of diabetes mellitus on in-hospital mortality in adult patients with COVID-19: a systematic review and meta-analysis
Halla Kaminska, Lukasz Szarpak, Dariusz Kosior, Wojciech Wieczorek, Agnieszka Szarpak, Mahdi Al-Jeabory, Wladyslaw Gawel, Aleksandra Gasecka, Milosz J. Jaguszewski, Przemyslawa Jarosz-Chobot
Acta Diabetologica.2021; 58(8): 1101. CrossRef - Risk phenotypes of diabetes and association with COVID-19 severity and death: a living systematic review and meta-analysis
Sabrina Schlesinger, Manuela Neuenschwander, Alexander Lang, Kalliopi Pafili, Oliver Kuss, Christian Herder, Michael Roden
Diabetologia.2021; 64(7): 1480. CrossRef - Evolution of a Cohort of COVID-19 Infection Suspects Followed-Up from Primary Health Care
Valle Coronado-Vázquez, Maria del Valle Ramírez-Durán, Juan Gómez-Salgado, María Silvia Dorado-Rabaneda, Elena Benito-Alonso, Marina Holgado-Juan, Cristina Bronchalo-González
Journal of Personalized Medicine.2021; 11(6): 459. CrossRef - Efficacy and safety of dulaglutide 3.0 and 4.5 mg in patients aged younger than 65 and 65 years or older: Post hoc analysis of the AWARD‐11 trial
Juan P. Frias, Enzo Bonora, Luis Nevárez Ruiz, Stanley H. Hsia, Heike Jung, Sohini Raha, David A. Cox, M. Angelyn Bethel, Manige Konig
Diabetes, Obesity and Metabolism.2021; 23(10): 2279. CrossRef - Renin‐Angiotensin Aldosterone System Inhibitors in Primary Prevention and COVID‐19
Jordan Loader, Erik Lampa, Stefan Gustafsson, Thomas Cars, Johan Sundström
Journal of the American Heart Association.2021;[Epub] CrossRef - Predictive value of HbA1c for in-hospital adverse prognosis in COVID-19: A systematic review and meta-analysis
Zheng Zhu, Yaqian Mao, Gang Chen
Primary Care Diabetes.2021; 15(6): 910. CrossRef - High Fibrosis-4 Index Is Related with Worse Clinical Outcome in Patients with Coronavirus Disease 2019 and Diabetes Mellitus: A Multicenter Observational Study
Sung-Woo Kim, Jae-Han Jeon, Jun Sung Moon, Mi Kyung Kim
Endocrinology and Metabolism.2021; 36(4): 800. CrossRef - COVID-19 Vaccination for Endocrine Patients: A Position Statement from the Korean Endocrine Society
Cheol Ryong Ku, Kyong Yeun Jung, Chang Ho Ahn, Jun Sung Moon, Ju Hee Lee, Eun Heui Kim, Hyemi Kwon, Hee Kyung Kim, Sunghwan Suh, Sangmo Hong, Jeonghoon Ha, Eun Roh, Jin Hwa Kim, Mi-kyung Kim
Endocrinology and Metabolism.2021; 36(4): 757. CrossRef - A Systematic Review and Meta-analysis of Diabetes Associated Mortality in Patients with COVID-19
Puneeta Gupta, Meeta Gupta, Neena KAtoch, Ketan Garg, Bhawna Garg
International Journal of Endocrinology and Metabolism.2021;[Epub] CrossRef - Diabetes, Drug Treatment, and Mortality in COVID-19: A Multinational Retrospective Cohort Study
Jennifer E. Nyland, Nazia T. Raja-Khan, Kerstin Bettermann, Philippe A. Haouzi, Douglas L. Leslie, Jennifer L. Kraschnewski, Leslie J. Parent, Patricia Sue Grigson
Diabetes.2021; 70(12): 2903. CrossRef - Impact of Diabetes on COVID-19 Mortality and Hospital Outcomes, a Global Perspective: An ONTOP Systematic Review and Meta-Analysis
Stavroula Kastora, Manisha Patel, Ben Carter, Mirela Delibegovic, Phyo Kyaw Myint
SSRN Electronic Journal .2021;[Epub] CrossRef - Response: Acute Hyperglycemic Crises with Coronavirus Disease-19: Case Reports (Diabetes Metab J 2020;44:349–53)
Na-young Kim, Eunyeong Ha, Jun Sung Moon, Yong-Hoon Lee, Eun Young Choi
Diabetes & Metabolism Journal.2020; 44(3): 484. CrossRef - Diabetes Mellitus is Associated with Severe Infection and Mortality in Patients with COVID-19: A Systematic Review and Meta-analysis
Luxiang Shang, Mengjiao Shao, Qilong Guo, Jia Shi, Yang Zhao, Jiasuoer Xiaokereti, Baopeng Tang
Archives of Medical Research.2020; 51(7): 700. CrossRef - Clinical Characteristics and Mortality Predictors of COVID-19 Patients Hospitalized at Nationally-Designated Treatment Hospitals
Seong-Su Moon, Kwan Lee, Jungi Park, Seongcheol Yun, Yun Sik Lee, Dong Seok Lee
Journal of Korean Medical Science.2020;[Epub] CrossRef - Mortality Rate and Predictors of Mortality in Hospitalized COVID-19 Patients with Diabetes
Dilaram Acharya, Kwan Lee, Dong Seok Lee, Yun Sik Lee, Seong-Su Moon
Healthcare.2020; 8(3): 338. CrossRef - Letter: The Risk of Diabetes on Clinical Outcomes in Patients with Coronavirus Disease 2019: A Retrospective Cohort Study (Diabetes Metab J 2020;44:405–13)
So-Yeon Kim, Kyung-Soo Kim
Diabetes & Metabolism Journal.2020; 44(4): 621. CrossRef - Response: The Risk of Diabetes on Clinical Outcomes in Patients with Coronavirus Disease 2019: A Retrospective Cohort Study (Diabetes Metab J 2020;44:405–13)
Seung Min Chung, June Hong Ahn, Jun Sung Moon
Diabetes & Metabolism Journal.2020; 44(4): 625. CrossRef - The Clinical Characteristics and Outcomes of Patients with Moderate-to-Severe Coronavirus Disease 2019 Infection and Diabetes in Daegu, South Korea
Mi Kyung Kim, Jae-Han Jeon, Sung-Woo Kim, Jun Sung Moon, Nan Hee Cho, Eugene Han, Ji Hong You, Ji Yeon Lee, Miri Hyun, Jae Seok Park, Yong Shik Kwon, Yeon-Kyung Choi, Ki Tae Kwon, Shin Yup Lee, Eon Ju Jeon, Jin-Woo Kim, Hyo-Lim Hong, Hyun Hee Kwon, Chi Yo
Diabetes & Metabolism Journal.2020; 44(4): 602. CrossRef - Fasting Plasma Glucose Level Independently Predicts the Mortality of Patients with Coronavirus Disease 2019 Infection: A Multicenter, Retrospective Cohort Study
Min Cheol Chang, Jong-Moon Hwang, Jae-Han Jeon, Sang Gyu Kwak, Donghwi Park, Jun Sung Moon
Endocrinology and Metabolism.2020; 35(3): 595. CrossRef - Diabetes Mellitus and COVID-19
Jeong Hyun Park
The Journal of Korean Diabetes.2020; 21(3): 116. CrossRef - Management of Diabetes in Coronavirus Disease 2019: Prognosis and Practical Issues
Hye Soon Kim
The Journal of Korean Diabetes.2020; 21(3): 120. CrossRef - Independent Impact of Diabetes on the Severity of Coronavirus Disease 2019 in 5,307 Patients in South Korea: A Nationwide Cohort Study
Sun Joon Moon, Eun-Jung Rhee, Jin-Hyung Jung, Kyung-Do Han, Sung-Rae Kim, Won-Young Lee, Kun-Ho Yoon
Diabetes & Metabolism Journal.2020; 44(5): 737. CrossRef - Adverse impact of renin–angiotensin system blockade on the clinical course in hospitalized patients with severe COVID-19: a retrospective cohort study
Jeong-Hoon Lim, Jang-Hee Cho, Yena Jeon, Ji Hye Kim, Ga Young Lee, Soojee Jeon, Hee Won Noh, Yong-Hoon Lee, Jaehee Lee, Hyun-Ha Chang, Hee-Yeon Jung, Ji-Young Choi, Sun-Hee Park, Chan-Duck Kim, Yong-Lim Kim, Shin-Woo Kim
Scientific Reports.2020;[Epub] CrossRef - Coronavirus Disease 2019 and Diabetes: The Epidemic and the Korean Diabetes Association Perspective
Junghyun Noh, Hyun-Ha Chang, In-Kyung Jeong, Kun Ho Yoon
Diabetes & Metabolism Journal.2020; 44(3): 372. CrossRef - Diabetes and COVID-19: Global and regional perspectives
In-Kyung Jeong, Kun Ho Yoon, Moon Kyu Lee
Diabetes Research and Clinical Practice.2020; 166: 108303. CrossRef
- Adult-Onset Type 1 Diabetes Development Following COVID-19 mRNA Vaccination
- Epidemiology
- The Changes of Trends in the Diagnosis and Treatment of Diabetic Foot Ulcer over a 10-Year Period: Single Center Study
- Choong Hee Kim, Jun Sung Moon, Seung Min Chung, Eun Jung Kong, Chul Hyun Park, Woo Sung Yoon, Tae Gon Kim, Woong Kim, Ji Sung Yoon, Kyu Chang Won, Hyoung Woo Lee
- Diabetes Metab J. 2018;42(4):308-319. Published online April 27, 2018
- DOI: https://doi.org/10.4093/dmj.2017.0076
- 5,004 View
- 66 Download
- 8 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background This study aims to describe the trends in the severity and treatment modality of patients with diabetic foot ulcer (DFU) at a single tertiary referral center in Korea over the last 10 years and compare the outcomes before and after the introduction of a multidisciplinary diabetic foot team.
Methods In this retrospective observational study, electronic medical records of patients from years 2002 to 2015 at single tertiary referral center were reviewed. Based on the year of first admission, patients were assigned to a group either before or after the year 2012, the year the diabetes team launched.
Results Of the 338 patients with DFU, 229 were first admitted until the year 2011 (group A), while 109 were first admitted since the year 2012 (group B). Mean age was higher in group B, and ulcer size was larger than those of group A. Whereas duration of diabetes was longer in group B, glycemic control was improved (mean glycosylated hemoglobin, 9.48% vs. 8.50%). The proportion of minor lower extremity amputation (LEA) was increased, but length of hospital stay was decreased (73.7±79.6 days vs. 39.8±36.9 days). As critical ischemic limb increased, the proportion of major LEA was not decreased.
Conclusion Improved glycemic control, multidisciplinary strategies with prompt surgical treatment resulted in reduced length of hospital stay, but these measures did not reduce major LEAs. The increase in critical ischemic limb may have played a role in the unexpected outcome, and may suggest the need for increased vascular intervention strategies in DFU treatment.
-
Citations
Citations to this article as recorded by- Life expectancy of patients with diabetic foot sepsis post-lower extremity amputation at a regional hospital in a South African setting. A retrospective cohort study
Thoriso C. Mokoala, Vhusani Sididzha, Etsumang D. Molefe, Thifhelimbilu E. Luvhengo
The Surgeon.2024; 22(2): e109. CrossRef - Effect of a multidisciplinary team approach in patients with diabetic foot ulcers on major adverse limb events (MALEs): systematic review and meta-analysis for the development of the Italian guidelines for the treatment of diabetic foot syndrome
Marco Meloni, Laura Giurato, Luca Monge, Cesare Miranda, Alessia Scatena, Benedetta Ragghianti, Giovanni Antonio Silverii, Cristiana Vermigli, Alessandro De Cassai, Antonio Volpe, Rodolfo Tramonta, Gerardo Medea, Corrado Bordieri, Marco Falcone, Laura Ste
Acta Diabetologica.2024;[Epub] CrossRef - Effect of Percutaneous Endovascular Angioplasty Combined with Negative Pressure Drainage on the “One-Stop” Treatment of Ischemic Diabetic Foot Ulcer
Bo Dong, Xixu Wang, Wei Wang, Biao Hong, Jue Wang, Heng Wang, Yun Gu
Annals of Vascular Surgery.2023; 92: 272. CrossRef - A novel Canadian multidisciplinary acute care pathway for people hospitalised with a diabetic foot ulcer
Abdelrahman Zamzam, Ann‐Marie McLaren, Emily Ram, Muzammil H. Syed, Sreenath Rave, Suzanne H. Lu, Mohammed Al‐Omran, Charles de Mestral
International Wound Journal.2023; 20(8): 3331. CrossRef - Impact of multidisciplinary care of diabetic foot infections for inpatients at Campbelltown Hospital
Timothy Choi, Uchechukwu Levi Osuagwu, Chau Tran, Krupali Bulsari, David Simmons
BMC Health Services Research.2023;[Epub] CrossRef - Multigene Panel Testing in Turkish Hereditary Cancer Syndrome Patients
Esra ARSLAN ATES, Ayberk TURKYILMAZ, Ceren ALAVANDA, Ozlem YILDIRIM, Ahmet Ilter GUNEY
Medeniyet Medical Journal.2022; 37(2): 150. CrossRef - Prediabetes; Prevention and Management
Asad Ali Mughal, Syed Taha Abbas, Huma Asad, Muhammed Zubair, Nasir Ali Khan, Shehla Naseem, Muhammad Zaman Shaikh
Pakistan BioMedical Journal.2022; : 03. CrossRef - A systematic review of multidisciplinary teams to reduce major amputations for patients with diabetic foot ulcers
Jackson Musuuza, Bryn L. Sutherland, Suleyman Kurter, Prakash Balasubramanian, Christie M. Bartels, Meghan B. Brennan
Journal of Vascular Surgery.2020; 71(4): 1433. CrossRef - The Complexity of Diabetic Foot Management: From Common Care to Best Practice. The Italian Expert Opinion by Delphi Survey
Elisabetta Salutini, Enrico Brocco, Roberto Da Ros, Luca Monge, Luigi Uccioli, Roberto Anichini
The International Journal of Lower Extremity Wounds.2020; 19(1): 34. CrossRef - The effect of a multidisciplinary outpatient team approach on outcomes in diabetic foot care: a single center study
Eline Huizing, Michiel A. Schreve, Willemijn Kortmann, Jan P. Bakker, Jean-Paul P. M. de Vries, Çağdaş Ünlü
The Journal of Cardiovascular Surgery.2020;[Epub] CrossRef
- Life expectancy of patients with diabetic foot sepsis post-lower extremity amputation at a regional hospital in a South African setting. A retrospective cohort study
- Epidemiology
- Clinical Characteristics of People with Newly Diagnosed Type 2 Diabetes between 2015 and 2016: Difference by Age and Body Mass Index
- Kyoung Hwa Ha, Cheol Young Park, In Kyung Jeong, Hyun Jin Kim, Sang-Yong Kim, Won Jun Kim, Ji Sung Yoon, In Joo Kim, Dae Jung Kim, Sungrae Kim
- Diabetes Metab J. 2018;42(2):137-146. Published online February 14, 2018
- DOI: https://doi.org/10.4093/dmj.2018.42.2.137
- 5,355 View
- 80 Download
- 11 Web of Science
- 11 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background We evaluated the clinical characteristics of insulin resistance and β-cell dysfunction in newly diagnosed, drug-naive people with type 2 diabetes by analyzing nationwide cross-sectional data.
Methods We collected the clinical data of 912 participants with newly diagnosed diabetes from 83 primary care clinics and hospitals nationwide from 2015 to 2016. The presence of insulin resistance and β-cell dysfunction was defined as a homeostatic model assessment of insulin resistance (HOMA-IR) value ≥2.5 and fasting C-peptide levels <1.70 ng/mL, respectively.
Results A total of 75.1% and 22.6% of participants had insulin resistance and β-cell dysfunction, respectively. The proportion of participants with insulin resistance but no β-cell dysfunction increased, and the proportion of participants with β-cell dysfunction but no insulin resistance decreased as body mass index (BMI) increased. People diagnosed with diabetes before 40 years of age had significantly higher HOMA-IR and BMI than those diagnosed over 65 years of age (HOMA-IR, 5.0 vs. 3.0; BMI, 28.7 kg/m2 vs. 25.1 kg/m2). However, the β-cell function indices were lower in people diagnosed before 40 years of age than in those diagnosed after 65 years of age (homeostatic model assessment of β-cell function, 39.3 vs. 64.9; insulinogenic index, 10.3 vs. 18.7; disposition index, 0.15 vs. 0.25).
Conclusion We observed that the main pathogenic mechanism of type 2 diabetes is insulin resistance in participants with newly diagnosed type 2 diabetes. In addition, young adults with diabetes are more likely to have higher insulin resistance with obesity and have higher insulin secretory defect with severe hyperglycemia in the early period of diabetes than older populations.
-
Citations
Citations to this article as recorded by- A double‐blind, Randomized controlled trial on glucose‐lowering EFfects and safety of adding 0.25 or 0.5 mg lobeglitazone in type 2 diabetes patients with INadequate control on metformin and dipeptidyl peptidase‐4 inhibitor therapy: REFIND study
Soree Ryang, Sang Soo Kim, Ji Cheol Bae, Ji Min Han, Su Kyoung Kwon, Young Il Kim, Il Seong Nam‐Goong, Eun Sook Kim, Mi‐kyung Kim, Chang Won Lee, Soyeon Yoo, Gwanpyo Koh, Min Jeong Kwon, Jeong Hyun Park, In Joo Kim
Diabetes, Obesity and Metabolism.2022; 24(9): 1800. CrossRef - Apparent Insulin Deficiency in an Adult African Population With New-Onset Type 2 Diabetes
Davis Kibirige, Isaac Sekitoleko, Priscilla Balungi, William Lumu, Moffat J. Nyirenda
Frontiers in Clinical Diabetes and Healthcare.2022;[Epub] CrossRef - Rising Incidence of Diabetes in Young Adults in South Korea: A National Cohort Study
Hyun Ho Choi, Giwoong Choi, Hojun Yoon, Kyoung Hwa Ha, Dae Jung Kim
Diabetes & Metabolism Journal.2022; 46(5): 803. CrossRef - A Real-World Study of Long-Term Safety and Efficacy of Lobeglitazone in Korean Patients with Type 2 Diabetes Mellitus
Bo-Yeon Kim, Hyuk-Sang Kwon, Suk Kyeong Kim, Jung-Hyun Noh, Cheol-Young Park, Hyeong-Kyu Park, Kee-Ho Song, Jong Chul Won, Jae Myung Yu, Mi Young Lee, Jae Hyuk Lee, Soo Lim, Sung Wan Chun, In-Kyung Jeong, Choon Hee Chung, Seung Jin Han, Hee-Seok Kim, Ju-Y
Diabetes & Metabolism Journal.2022; 46(6): 855. CrossRef - The Potential Effect of Rhizoma coptidis on Polycystic Ovary Syndrome Based on Network Pharmacology and Molecular Docking
Liyun Duan, De Jin, Xuedong An, Yuehong Zhang, Shenghui Zhao, Rongrong Zhou, Yingying Duan, Yuqing Zhang, Xinmin Liu, Fengmei Lian, Wen yi Kang
Evidence-Based Complementary and Alternative Medicine.2021; 2021: 1. CrossRef - PRKAA2variation and the clinical characteristics of patients newly diagnosed with type 2 diabetes mellitus in Yogyakarta, Indonesia
Dita Maria Virginia, Mae Sri Hartati Wahyuningsih, Dwi Aris Agung Nugrahaningsih
Asian Biomedicine.2021; 15(4): 161. CrossRef - Efficacy and Safety of Pioglitazone versus Glimepiride after Metformin and Alogliptin Combination Therapy: A Randomized, Open-Label, Multicenter, Parallel-Controlled Study
Jeong Mi Kim, Sang Soo Kim, Jong Ho Kim, Mi Kyung Kim, Tae Nyun Kim, Soon Hee Lee, Chang Won Lee, Ja Young Park, Eun Sook Kim, Kwang Jae Lee, Young Sik Choi, Duk Kyu Kim, In Joo Kim
Diabetes & Metabolism Journal.2020; 44(1): 67. CrossRef - Favorable Glycemic Control with Once-Daily Insulin Degludec/Insulin Aspart after Changing from Basal Insulin in Adults with Type 2 Diabetes
Han Na Jang, Ye Seul Yang, Seong Ok Lee, Tae Jung Oh, Bo Kyung Koo, Hye Seung Jung
Endocrinology and Metabolism.2019; 34(4): 382. CrossRef - Insulin Resistance versus β-Cell Failure: Is It Changing in Koreans?
Mi-kyung Kim
Diabetes & Metabolism Journal.2018; 42(2): 128. CrossRef - Response: Clinical Characteristics of People with Newly Diagnosed Type 2 Diabetes between 2015 and 2016: Difference by Age and Body Mass Index (Diabetes Metab J2018;42:137-46)
Kyoung Hwa Ha, Dae Jung Kim, Sungrae Kim
Diabetes & Metabolism Journal.2018; 42(3): 251. CrossRef - Letter: Clinical Characteristics of People with Newly Diagnosed Type 2 Diabetes between 2015 and 2016: Difference by Age and Body Mass Index (Diabetes Metab J 2018;42:137-46)
Ah Reum Khang
Diabetes & Metabolism Journal.2018; 42(3): 249. CrossRef
- A double‐blind, Randomized controlled trial on glucose‐lowering EFfects and safety of adding 0.25 or 0.5 mg lobeglitazone in type 2 diabetes patients with INadequate control on metformin and dipeptidyl peptidase‐4 inhibitor therapy: REFIND study
- Response: Predicting Mortality of Critically Ill Patients by Blood Glucose Levels (
Diabetes Metab J 2013;37:385-90) - Byung Sam Park, Ji Sung Yoon
- Diabetes Metab J. 2014;38(1):81-82. Published online February 19, 2014
- DOI: https://doi.org/10.4093/dmj.2014.38.1.81
- 2,787 View
- 24 Download
- Relative Skeletal Muscle Mass Is Associated with Development of Metabolic Syndrome
- Byung Sam Park, Ji Sung Yoon
- Diabetes Metab J. 2013;37(6):458-464. Published online December 12, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.6.458
- 5,629 View
- 104 Download
- 73 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Visceral adiposity is related to insulin resistance. Skeletal muscle plays a central role in insulin-mediated glucose disposal; however, little is known about the association between muscle mass and metabolic syndrome (MS). This study is to clarify the clinical role of skeletal muscle mass in development of MS.
Methods A total of 1,042 subjects were enrolled. Subjects with prior MS and chronic diseases were excluded. After 24 months, development of MS was assessed using NCEP-ATP III criteria. Skeletal muscle mass (SMM; kg), body fat mass (BFM; kg), and visceral fat area (VFA; cm2) were obtained from bioelectrical analysis. Then, the following values were calculated as follows: percent of SMM (SMM%; %): SMM (kg)/weight (kg), skeletal muscle index (SMI; kg/m2): SMM (kg)/height (m2), skeletal muscle to body fat ratio (MFR): SMM (kg)/BFM (kg), and skeletal muscle to visceral fat ratio (SVR; kg/cm2): SMM (kg)/VFA (cm2).
Results Among 838 subjects, 88 (10.5%) were newly diagnosed with MS. Development of MS increased according to increasing quintiles of BMI, SMM, VFA, and SMI, but was negatively associated with SMM%, MFR, and SVR. VFA was positively associated with high waist circumference (WC), high blood pressure (BP), dysglycemia, and high triglyceride (TG). In contrast, MFR was negatively associated with high WC, high BP, dysglycemia, and high TG. SVR was negatively associated with all components of MS.
Conclusion Relative SMM ratio to body composition, rather than absolute mass, may play a critical role in development of MS and could be used as a strong predictor.
-
Citations
Citations to this article as recorded by- Relationship between adiponectin and muscle mass in patients with metabolic syndrome and obesity
Daniel de Luis, David Primo, Olatz Izaola, Juan José Lopez Gomez
Journal of Diabetes and its Complications.2024; 38(4): 108706. CrossRef - The longitudinal association of adipose-to-lean ratio with incident cardiometabolic morbidity: The CARDIA study
Robert Booker, Mandy Wong, Michael P. Bancks, Mercedes R. Carnethon, Lisa S. Chow, Cora E. Lewis, Pamela J. Schreiner, Shaina J. Alexandria
Journal of Diabetes and its Complications.2024; 38(5): 108725. CrossRef - Assessing Sarcopenic Obesity Risk in Children During the COVID-19 Pandemic: Grip-to-BMI Ratio
Bahar Öztelcan Gündüz, Aysu Duyan Çamurdan, Mücahit Yıldız, F. Nur Baran Aksakal, Emine Nüket Ünsal
Medical Research Reports.2024; 7(1): 18. CrossRef - Sex differences in body composition in youth with type 1 diabetes and its predictive value in cardiovascular disease risk assessment
Avivit Brener, Sandy Hamama, Hagar Interator, Asaf Ben Simon, Irina Laurian, Anna Dorfman, Efrat Chorna, Michal Yackobovitch‐Gavan, Asaf Oren, Ori Eyal, Yael Lebenthal
Diabetes/Metabolism Research and Reviews.2023;[Epub] CrossRef - Epidemiological, mechanistic, and practical bases for assessment of cardiorespiratory fitness and muscle status in adults in healthcare settings
Jaime A. Gallo-Villegas, Juan C. Calderón
European Journal of Applied Physiology.2023; 123(5): 945. CrossRef - The Effect of Childhood Obesity or Sarcopenic Obesity on Metabolic Syndrome Risk in Adolescence: The Ewha Birth and Growth Study
Hyunjin Park, Seunghee Jun, Hye-Ah Lee, Hae Soon Kim, Young Sun Hong, Hyesook Park
Metabolites.2023; 13(1): 133. CrossRef - Relationships of BMI, muscle-to-fat ratio, and handgrip strength-to-BMI ratio to physical fitness in Spanish children and adolescents
Samuel Manzano-Carrasco, Jorge Garcia-Unanue, Eero A. Haapala, Jose Luis Felipe, Leonor Gallardo, Jorge Lopez-Fernandez
European Journal of Pediatrics.2023; 182(5): 2345. CrossRef - Body physique rating as a factor to identify at-risk Mexicans for Metabolic Syndrome
Oscar Herrera-Fomperosa, Sergio K. Bustamante-Villagomez, Sarahí Vazquez-Álvarez, Gabriela Vázquez-Marroquín, Leonardo M. Porchia, Enrique Torres-Rasgado, Ricardo Pérez-Fuentes, M. Elba Gonzalez-Mejia
Human Nutrition & Metabolism.2023; 33: 200206. CrossRef - The association between creatinine to body weight ratio and the risk of progression to diabetes from pre-diabetes: a 5-year cohort study in Chinese adults
Tong Li, Changchun Cao, Xuan Xuan, Wenjing Liu, Xiaohua Xiao, Cuimei Wei
BMC Endocrine Disorders.2023;[Epub] CrossRef - Muscle-to-Fat Ratio for Predicting Metabolic Syndrome Components in Children with Overweight and Obesity
Noga Salton, Sharona Kern, Hagar Interator, Adar Lopez, Hadar Moran-Lev, Yael Lebenthal, Avivit Brener
Childhood Obesity.2022; 18(2): 132. CrossRef - Mentale Gesundheit und physische Aktivität
Wolfgang Laube
Manuelle Medizin.2022; 60(1): 13. CrossRef - Increased odds of having the metabolic syndrome with greater fat‐free mass: counterintuitive results from the National Health and Nutrition Examination Survey database
Jean‐Christophe Lagacé, Alexis Marcotte‐Chenard, Jasmine Paquin, Dominic Tremblay, Martin Brochu, Isabelle J. Dionne
Journal of Cachexia, Sarcopenia and Muscle.2022; 13(1): 377. CrossRef - Lipoprotein subfractions in patients with sarcopenia and their relevance to skeletal muscle mass and function
Hui Gong, Yang Liu, Xing Lyu, Lini Dong, Xiangyu Zhang
Experimental Gerontology.2022; 159: 111668. CrossRef - Health Risks of Sarcopenic Obesity in Overweight Children and Adolescents: Data from the CHILT III Programme (Cologne)
Carolin Sack, Nina Ferrari, David Friesen, Fabiola Haas, Marlen Klaudius, Lisa Schmidt, Gabriel Torbahn, Hagen Wulff, Christine Joisten
Journal of Clinical Medicine.2022; 11(1): 277. CrossRef - Creatinine-to-body weight ratio is a predictor of incident diabetes: a population-based retrospective cohort study
Jiacheng He
Diabetology & Metabolic Syndrome.2022;[Epub] CrossRef - Relative low muscle mass and muscle strength is associated with the prevalence of metabolic syndrome in patients with type 2 diabetes
Maya Takegami, Yoshitaka Hashimoto, Masahide Hamaguchi, Ayumi Kaji, Ryosuke Sakai, Takuro Okamura, Noriyuki Kitagawa, Takafumi Osaka, Hiroshi Okada, Naoko Nakanishi, Saori Majima, Takafumi Senmaru, Emi Ushigome, Mai Asano, Masahiro Yamazaki, Michiaki Fuku
Journal of Clinical Biochemistry and Nutrition.2022; 71(2): 136. CrossRef - “Big Data” Approaches for Prevention of the Metabolic Syndrome
Xinping Jiang, Zhang Yang, Shuai Wang, Shuanglin Deng
Frontiers in Genetics.2022;[Epub] CrossRef - Teil 2: Muskeldysfunktionen – mit Training gegen Schmerz
Wolfgang Laube
Manuelle Medizin.2022; 60(3): 129. CrossRef - Impact of Low Skeletal Muscle Mass and Obesity on Hearing Loss in Asymptomatic Individuals: A Population-Based Study
Chul-Hyun Park, Kyung Jae Yoon, Yong-Taek Lee, Sung Min Jin, Sang Hyuk Lee, Tae Hwan Kim
Healthcare.2022; 10(10): 2022. CrossRef - Physical activity level, sitting time, and skeletal muscle mass between esports players and non-esports players
Zhi H. SEE, Mohamad S. ABDUL HAMID
Gazzetta Medica Italiana Archivio per le Scienze Mediche.2022;[Epub] CrossRef - Associations of changes in fat free mass with risk for type 2 diabetes: Hispanic Community Health Study/Study of Latinos
M.N. LeCroy, S. Hua, R.C. Kaplan, D. Sotres-Alvarez, Q. Qi, B. Thyagarajan, L.C. Gallo, A. Pirzada, M.L. Daviglus, N. Schneiderman, G.A. Talavera, C.R. Isasi
Diabetes Research and Clinical Practice.2021; 171: 108557. CrossRef - The phospholipase A2 family’s role in metabolic diseases: Focus on skeletal muscle
Iris Prunonosa Cervera, Brendan M. Gabriel, Peter Aldiss, Nicholas M. Morton
Physiological Reports.2021;[Epub] CrossRef - Bone Health in Aging Men: Does Zinc and Cuprum Level Matter?
Aleksandra Rył, Tomasz Miazgowski, Aleksandra Szylińska, Agnieszka Turoń-Skrzypińska, Alina Jurewicz, Andrzej Bohatyrewicz, Iwona Rotter
Biomolecules.2021; 11(2): 237. CrossRef - Animal Protein versus Plant Protein in Supporting Lean Mass and Muscle Strength: A Systematic Review and Meta-Analysis of Randomized Controlled Trials
Meng Thiam Lim, Bernice Jiaqi Pan, Darel Wee Kiat Toh, Clarinda Nataria Sutanto, Jung Eun Kim
Nutrients.2021; 13(2): 661. CrossRef - Effects of Exercise Intervention on Mitochondrial Stress Biomarkers in Metabolic Syndrome Patients: A Randomized Controlled Trial
Jae Seung Chang, Jun Namkung
International Journal of Environmental Research and Public Health.2021; 18(5): 2242. CrossRef - Association between sarcopenia level and metabolic syndrome
Su Hwan Kim, Ji Bong Jeong, Jinwoo Kang, Dong-Won Ahn, Ji Won Kim, Byeong Gwan Kim, Kook Lae Lee, Sohee Oh, Soon Ho Yoon, Sang Joon Park, Doo Hee Lee, Masaki Mogi
PLOS ONE.2021; 16(3): e0248856. CrossRef - Sarcopenia and Appendicular Muscle Mass as Predictors of Impaired Fasting Glucose/Type 2 Diabetes in Elderly Women
Carola Buscemi, Yvelise Ferro, Roberta Pujia, Elisa Mazza, Giada Boragina, Angela Sciacqua, Salvatore Piro, Arturo Pujia, Giorgio Sesti, Silvio Buscemi, Tiziana Montalcini
Nutrients.2021; 13(6): 1909. CrossRef - Low muscle mass in older adults and mortality: A systematic review and meta-analysis
Felipe M. de Santana, Melissa O. Premaor, Nicolas Y. Tanigava, Rosa M.R. Pereira
Experimental Gerontology.2021; 152: 111461. CrossRef - Association of obesity, visceral adiposity, and sarcopenia with an increased risk of metabolic syndrome: A retrospective study
Su Hwan Kim, Hyoun Woo Kang, Ji Bong Jeong, Dong Seok Lee, Dong-Won Ahn, Ji Won Kim, Byeong Gwan Kim, Kook Lae Lee, Sohee Oh, Soon Ho Yoon, Sang Joon Park, Mauro Lombardo
PLOS ONE.2021; 16(8): e0256083. CrossRef - Der Muskulatur mehr Aufmerksamkeit schenken!
Wolfgang Laube
Manuelle Medizin.2021; 59(4): 302. CrossRef - Dietary Protein Requirement Threshold and Micronutrients Profile in Healthy Older Women Based on Relative Skeletal Muscle Mass
Praval Khanal, Lingxiao He, Hans Degens, Georgina K. Stebbings, Gladys L. Onambele-Pearson, Alun G. Williams, Martine Thomis, Christopher I. Morse
Nutrients.2021; 13(9): 3076. CrossRef - Effects of different definitions of low muscle mass on its association with metabolic syndrome in older adults: A Korean nationwide study
Yerim Jeon, Ki Young Son
Geriatrics & Gerontology International.2021; 21(11): 1003. CrossRef - Musclin Is Related to Insulin Resistance and Body Composition, but Not to Body Mass Index or Cardiorespiratory Capacity in Adults
Yeliana L. Sánchez, Manuela Yepes-Calderón, Luis Valbuena, Andrés F. Milán, María C. Trillos-Almanza, Sergio Granados, Miguel Peña, Mauricio Estrada-Castrillón, Juan C. Aristizábal, Raúl Narvez-Sanchez, Jaime Gallo-Villegas, Juan C. Calderón
Endocrinology and Metabolism.2021; 36(5): 1055. CrossRef - Relative Lean Body Mass and Waist Circumference for the Identification of Metabolic Syndrome in the Korean General Population
Eunjoo Kwon, Eun-Hee Nah, Suyoung Kim, Seon Cho
International Journal of Environmental Research and Public Health.2021; 18(24): 13186. CrossRef - Impact of Skeletal Muscle Mass on Metabolic Health
Gyuri Kim, Jae Hyeon Kim
Endocrinology and Metabolism.2020; 35(1): 1. CrossRef - Skeletal muscle area and density are associated with lipid and lipoprotein cholesterol levels: The Multi-Ethnic Study of Atherosclerosis
Chantal A. Vella, Megan C. Nelson, Jonathan T. Unkart, Iva Miljkovic, Matthew A. Allison
Journal of Clinical Lipidology.2020; 14(1): 143. CrossRef - Creatinine/(cystatin C × body weight) ratio is associated with skeletal muscle mass index
Kensuke Nishida, Yoshitaka Hashimoto, Ayumi Kaji, Takuro Okamura, Ryousuke Sakai, Noriyuki Kitagawa, Takafumi Osaka, Masahide Hamaguchi, Michiaki Fukui
Endocrine Journal.2020; 67(7): 733. CrossRef - Testosterone Therapy for Prevention and Treatment of Obesity in Men
Monica Caliber, Farid Saad
Androgens: Clinical Research and Therapeutics.2020; 1(1): 40. CrossRef - Creatinine to Body Weight Ratio Is Associated with Incident Diabetes: Population-Based Cohort Study
Yoshitaka Hashimoto, Takuro Okamura, Masahide Hamaguchi, Akihiro Obora, Takao Kojima, Michiaki Fukui
Journal of Clinical Medicine.2020; 9(1): 227. CrossRef - Skeletal muscle – A bystander or influencer of metabolic syndrome?
Gina L. Richter-Stretton, Andrew S. Fenning, Rebecca K. Vella
Diabetes & Metabolic Syndrome: Clinical Research & Reviews.2020; 14(5): 867. CrossRef - Using relative handgrip strength to identify children at risk of sarcopenic obesity
Seryozha Gontarev, Mirko Jakimovski, Georgi Georgiev
Nutrición Hospitalaria.2020;[Epub] CrossRef - Nonalcoholic Fatty Liver Disease Is Associated With Low Skeletal Muscle Mass in Overweight/Obese Youths
Lucia Pacifico, Francesco Massimo Perla, Gianmarco Andreoli, Rosangela Grieco, Pasquale Pierimarchi, Claudio Chiesa
Frontiers in Pediatrics.2020;[Epub] CrossRef - Independent and combined associations of cardiorespiratory fitness and muscle strength with metabolic syndrome in older adults: A cross-sectional study
Marcyo Câmara, Rodrigo Alberto Vieira Browne, Gabriel Costa Souto, Daniel Schwade, Ludmila Pereira Lucena Cabral, Geovani Araújo Dantas Macêdo, Luiz Fernando Farias-Junior, Fabíola Leite Gouveia, Telma Maria Araújo Moura Lemos, Kenio Costa Lima, Todd A. D
Experimental Gerontology.2020; 135: 110923. CrossRef - A counterintuitive perspective for the role of fat‐free mass in metabolic health
Jean‐Christophe Lagacé, Martin Brochu, Isabelle J. Dionne
Journal of Cachexia, Sarcopenia and Muscle.2020; 11(2): 343. CrossRef - Response: The way fat‐free mass is reported may change the conclusions regarding its protective effect on metabolic health
Jean‐Christophe Lagace, Martin Brochu, Isabelle J. Dionne
Clinical Endocrinology.2020; 92(1): 79. CrossRef - The Association between Major Dietary Pattern and Low Muscle Mass in Korean Middle-Aged and Elderly Populations: Based on the Korea National Health and Nutrition Examination Survey
Seong-Ah Kim, Jinwoo Ha, Byeonghwi Lim, Jun-Mo Kim, Sangah Shin
Nutrients.2020; 12(11): 3543. CrossRef - Total body skeletal muscle mass and diet in children aged 6–8 years: ANIVA Study
Maria Morales-Suarez-Varela, Isabel Peraita-Costa, Carlos Guillamon Escudero, Agustin Llopis-Morales, Agustin Llopis-Gonzalez
Applied Physiology, Nutrition, and Metabolism.2019; 44(9): 944. CrossRef - The way fat‐free mass is reported may change the conclusions regarding its protective effect on metabolic health
Jean‐Christophe Lagacé, Dominic Tremblay, Jasmine Paquin, Alexis Marcotte‐Chénard, Martin Brochu, Isabelle J. Dionne
Clinical Endocrinology.2019; 91(6): 903. CrossRef - Components of Metabolic Syndrome in Korean Adults: A Hospital-Based Cohort at Seoul National University Bundang Hospital
Soo Lim, Se Hee Min, Ji Hyun Lee, Lee Kyung Kim, Dong-Hwa Lee, Jie-Eun Lee, Kyoung Min Kim, Sunmi Lee, Kyoung-Chan Park, Yun Jong Lee
Journal of Obesity & Metabolic Syndrome.2019; 28(2): 118. CrossRef - Skeletal muscle as a protagonist in the pregnancy metabolic syndrome
Raul Narvaez-Sanchez, Juan C. Calderón, Gloria Vega, Maria Camila Trillos, Sara Ospina
Medical Hypotheses.2019; 126: 26. CrossRef - Increase in relative skeletal muscle mass over time and its inverse association with metabolic syndrome development: a 7-year retrospective cohort study
Gyuri Kim, Seung-Eun Lee, Ji Eun Jun, You-Bin Lee, Jiyeon Ahn, Ji Cheol Bae, Sang-Man Jin, Kyu Yeon Hur, Jae Hwan Jee, Moon-Kyu Lee, Jae Hyeon Kim
Cardiovascular Diabetology.2018;[Epub] CrossRef - Association of Age-Related Trends in Blood Pressure and Body Composition Indices in Healthy Adults
Wei Li, Yan He, Lili Xia, Xinghua Yang, Feng Liu, Jingang Ma, Zhiping Hu, Yajun Li, Dongxue Li, Jiajia Jiang, Guangliang Shan, Changlong Li
Frontiers in Physiology.2018;[Epub] CrossRef - Metabolic syndrome and body shape predict differences in health parameters in farm working women
Ilze Mentoor, Maritza Kruger, Theo Nell
BMC Public Health.2018;[Epub] CrossRef - Associations of stunting in early childhood with cardiometabolic risk factors in adulthood
Emanuella De Lucia Rolfe, Giovanny Vinícius Araújo de França, Carolina Avila Vianna, Denise P. Gigante, J. Jaime Miranda, John S. Yudkin, Bernardo Lessa Horta, Ken K. Ong, C. Mary Schooling
PLOS ONE.2018; 13(4): e0192196. CrossRef - Relationship Between Relative Skeletal Muscle Mass and Nonalcoholic Fatty Liver Disease: A 7‐Year Longitudinal Study
Gyuri Kim, Seung‐Eun Lee, You‐Bin Lee, Ji Eun Jun, Jiyeon Ahn, Ji Cheol Bae, Sang‐Man Jin, Kyu Yeon Hur, Jae Hwan Jee, Moon‐Kyu Lee, Jae Hyeon Kim
Hepatology.2018; 68(5): 1755. CrossRef - Relationships among Skeletal Muscle Mass, Health Related Factors, Nutrient Intake, and Physical Activities in Male Adolescents: Based on the 5th (2009-2011) Korean National Health and Nutrition Examination Survey (KNHANES)
In-Kyung Jung, Jung-Hyun Kim
The Korean Journal of Community Living Science.2018; 29(2): 185. CrossRef - Using relative handgrip strength to identify children at risk of sarcopenic obesity
Michal Steffl, Jan Chrudimsky, James J. Tufano, Masaki Mogi
PLOS ONE.2017; 12(5): e0177006. CrossRef - International society of sports nutrition position stand: diets and body composition
Alan A. Aragon, Brad J. Schoenfeld, Robert Wildman, Susan Kleiner, Trisha VanDusseldorp, Lem Taylor, Conrad P. Earnest, Paul J. Arciero, Colin Wilborn, Douglas S. Kalman, Jeffrey R. Stout, Darryn S. Willoughby, Bill Campbell, Shawn M. Arent, Laurent Banno
Journal of the International Society of Sports Nutrition.2017;[Epub] CrossRef - Relationship between rectus abdominis muscle thickness and metabolic syndrome in middle-aged men
Eun Sil Choi, Soo Hyun Cho, Jung-Ha Kim, Etsuro Ito
PLOS ONE.2017; 12(9): e0185040. CrossRef - Health-related quality of life and activity limitation in an elderly Korean population with sarcopenia: The Fourth Korea National Health and Nutrition Examination Survey (KNHANES IV-2, 3), 2008–2009
T.H. Kim, S.-H. Kim, J. Kim, H.-J. Hwang
European Geriatric Medicine.2017; 8(4): 360. CrossRef - Differential association between sarcopenia and metabolic phenotype in Korean young and older adults with and without obesity
You‐Cheol Hwang, In‐Jin Cho, In‐Kyung Jeong, Kyu Jeung Ahn, Ho Yeon Chung
Obesity.2017; 25(1): 244. CrossRef - Reference Values of Skeletal Muscle Mass for Korean Children and Adolescents Using Data from the Korean National Health and Nutrition Examination Survey 2009-2011
Kirang Kim, Sangmo Hong, Eun Young Kim, Bin He
PLOS ONE.2016; 11(4): e0153383. CrossRef - Insulin sensitivity, body composition and adipose depots following 12 w combined endurance and strength training in dysglycemic and normoglycemic sedentary men
Torgrim Mikal Langleite, Jørgen Jensen, Frode Norheim, Hanne Løvdal Gulseth, Daniel Steensen Tangen, Kristoffer Jensen Kolnes, Ansgar Heck, Tryggve Storås, Guro Grøthe, Marius Adler Dahl, Anders Kielland, Torgeir Holen, Hans Jørgen Noreng, Hans Kristian S
Archives of Physiology and Biochemistry.2016; 122(4): 167. CrossRef - Association between fat free mass and glucose homeostasis: Common knowledge revisited
Karine Perreault, Jean-Christophe Lagacé, Martin Brochu, Isabelle J. Dionne
Ageing Research Reviews.2016; 28: 46. CrossRef - Low skeletal muscle mass is associated with non-alcoholic fatty liver disease in Korean adults: the Fifth Korea National Health and Nutrition Examination Survey
Hee Yeon Kim, Chang Wook Kim, Chung-Hwa Park, Jong Young Choi, Kyungdo Han, Anwar T Merchant, Yong-Moon Park
Hepatobiliary & Pancreatic Diseases International.2016; 15(1): 39. CrossRef - The ratio of skeletal muscle mass to visceral fat area is a main determinant linking circulating irisin to metabolic phenotype
You-Cheol Hwang, Won Seon Jeon, Cheol-Young Park, Byung-Soo Youn
Cardiovascular Diabetology.2016;[Epub] CrossRef - Effects of a weight loss program on body composition and the metabolic profile in obese postmenopausal women displaying various obesity phenotypes: a MONET group study
Eve Normandin, Eric Doucet, Rémi Rabasa-Lhoret, Martin Brochu
Applied Physiology, Nutrition, and Metabolism.2015; 40(7): 695. CrossRef - Analytic morphomics identifies predictors of new‐onset diabetes after liver transplantation
Valerie M. Vaughn, David C. Cron, Michael N. Terjimanian, Zachary S. Gala, Stewart C. Wang, Grace L. Su, Michael L. Volk
Clinical Transplantation.2015; 29(5): 458. CrossRef - Reduced Flexibility Associated with Metabolic Syndrome in Community-Dwelling Elders
Ke-Vin Chang, Chen-Yu Hung, Chia-Ming Li, Yu-Hung Lin, Tyng-Guey Wang, Keh-Sung Tsai, Der-Sheng Han, Diego Fraidenraich
PLOS ONE.2015; 10(1): e0117167. CrossRef - Metabolic risk factors in U.S. youth with low relative muscle mass
Sunkyung Kim, Rodolfo Valdez
Obesity Research & Clinical Practice.2015; 9(2): 125. CrossRef - Comparison of waist to height ratio and body indices for prediction of metabolic disturbances in the Korean population: the Korean National Health and Nutrition Examination Survey 2008–2011
Seok Hui Kang, Kyu Hyang Cho, Jong Won Park, Jun Young Do
BMC Endocrine Disorders.2015;[Epub] CrossRef - N-3 fatty acid intake altered fat content and fatty acid distribution in chicken breast muscle, but did not influence mRNA expression of lipid-related enzymes
Anna Haug, Nicole F Nyquist, Magny Thomassen, Arne T Høstmark, Tone-Kari Knutsdatter Østbye
Lipids in Health and Disease.2014;[Epub] CrossRef - Métodos de análise da composição corporal em adultos obesos
Rávila Graziany Machado de Souza, Aline Corado Gomes, Carla Marques Maia do Prado, João Felipe Mota
Revista de Nutrição.2014; 27(5): 569. CrossRef
- Relationship between adiponectin and muscle mass in patients with metabolic syndrome and obesity
- Diabetogenic Effect of Statins: A Double-Edged Sword?
- Ji Sung Yoon, Hyoung Woo Lee
- Diabetes Metab J. 2013;37(6):415-422. Published online December 12, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.6.415
- 3,619 View
- 43 Download
- 16 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Statins are widely prescribed cholesterol-lowering agents, which have been demonstrated to significantly reduce cardiovascular morbidity and mortality. However, recent trials have reported that statins cause worsening of hyperglycemia and increase the risk of new-onset diabetes. The association between the diabetogenic effect of statins with intensive dose and accompanying major risk factors for diabetes has been demonstrated. However, statins do not appear to have a class effect on insulin sensitivity in non-diabetic patients. Numerous mechanisms have been suggested to explain how statins cause β-cell insulin secretory dysfunction and peripheral insulin resistance leading to incident diabetes. According to findings from an aggregate of large clinical trials, the benefits of statin treatment appear to outweigh the risk of new-onset diabetes. Therefore, it would be inappropriate to discontinue the use of statins for prevention of cardiovascular events because of its potential risk for development of incident diabetes. This review addresses the currently available evidence related to statin use and new-onset diabetes from a clinical perspective.
-
Citations
Citations to this article as recorded by- High doses of rosuvastatin induce impaired branched‐chain amino acid catabolism and lead to insulin resistance
Xue Bai, Xingzhen Long, Fang Song, Baolin Chen, Changcheng Sheng, Cailin Tang, Li Li, Jiaxing Zhang, Rui Zhang, Jiquan Zhang, Jiali Li
Experimental Physiology.2023; 108(7): 961. CrossRef - Statins and the diabetogenic effect (II)
Nicolae Bacinschi, Ina Guţu, Anastasia Caracaş, Svetlana Latuş, Stela Bacinschi-Gheorghiţă, Aurelia Bacinschi, Dumitru Ştîrba, Olesea Malancea
Farmacist.ro.2022; 5(208): 14. CrossRef - Statins and the diabetogenic effect (I)
Nicolae Bacinschi, Ina Guţu, Anastasia Caracaş, Svetlana Latuş, Stela Bacinschi-Gheorghiţă, Aurelia Bacinschi, Dumitru Ştîrba, Olesea Malancea
Farmacist.ro.2022; 4(207): 16. CrossRef - Efficacy and Safety of a Fixed-Dose Combination of Candesartan and Rosuvastatin on Blood Pressure and Cholesterol in Patients With Hypertension and Hypercholesterolemia: A Multicenter, Randomized, Double-Blind, Parallel Phase III Clinical Study
Kyoung Im Cho, Bo Hyun Kim, Yong Hyun Park, Jeong-Cheon Ahn, Sang Hyun Kim, Wook Jin Chung, Weon Kim, Il Suk Sohn, Jin Ho Shin, Yong Jin Kim, Kiyuk Chang, Cheol Woong Yu, Soe Hee Ahn, Seok Yeon Kim, Jae Kean Ryu, Jong Young Lee, Bum Kee Hong, Taek Jong Ho
Clinical Therapeutics.2019; 41(8): 1508. CrossRef - Change in ALT levels after administration of HMG‐CoA reductase inhibitors to subjects with pretreatment levels three times the upper normal limit in clinical practice
Hyunah Kim, Hyeseon Lee, Tong Min Kim, So Jung Yang, Seo Yeon Baik, Seung‐Hwan Lee, Jae‐Hyoung Cho, Hyunyong Lee, Hyeon Woo Yim, In Young Choi, Kun‐Ho Yoon, Hun‐Sung Kim
Cardiovascular Therapeutics.2018;[Epub] CrossRef - Phenotyping of Korean patients with better-than-expected efficacy of moderate-intensity statins using tensor factorization
Jingyun Choi, Yejin Kim, Hun-Sung Kim, In Young Choi, Hwanjo Yu, Katriina Aalto-Setala
PLOS ONE.2018; 13(6): e0197518. CrossRef - Management of patients with statin intolerance
Sabine Fischer, Ulrich Julius
Atherosclerosis Supplements.2017; 30: 33. CrossRef - Use of Moderate‐Intensity Statins for Low‐Density Lipoprotein Cholesterol Level above 190 mg/dL at Baseline in Koreans
Hun‐Sung Kim, Hyeseon Lee, Sue Hyun Lee, Yoo Jin Jeong, Tong Min Kim, So Jung Yang, Sun Jung Baik, Hyunah Kim, Seung‐Hwan Lee, Jae Hyoung Cho, In‐Young Choi, Kun‐Ho Yoon, Ju Han Kim
Basic & Clinical Pharmacology & Toxicology.2017; 121(4): 272. CrossRef - Uso de estatinas e o risco de Diabetes Mellitus tipo 2: Revisão Baseada na Evidência
Susana Silva, Nuno Monteiro
Revista Brasileira de Medicina de Família e Comunidade.2016; 11(38): 1. CrossRef - Association of statin use and stress-induced hyperglycemia in patients with acute ST-elevation myocardial infarction
Chen Yan, Ma Qin, Yang S Juan, Li Y Tao, Gao M dong, Zeng Zechun, Yang X Chun, Cong H Liang, Liu Yin, Meng Kang
JRSM Cardiovascular Disease.2016; 5: 204800401663944. CrossRef - Statin‐related aminotransferase elevation according to baseline aminotransferases level in real practice in Korea
H.‐S. Kim, S. H. Lee, H. Kim, S.‐H. Lee, J. H. Cho, H. Lee, H. W. Yim, S.‐H. Kim, I.‐Y. Choi, K.‐H. Yoon, J. H. Kim
Journal of Clinical Pharmacy and Therapeutics.2016; 41(3): 266. CrossRef - Statins and their increased risk of inducing diabetes
Aris P Agouridis, Michael S Kostapanos, Moses S Elisaf
Expert Opinion on Drug Safety.2015; 14(12): 1835. CrossRef - Effects ofVacciniumBerries on Serum Lipids: A Meta-Analysis of Randomized Controlled Trials
Yitong Zhu, Ya Miao, Zheying Meng, Yuan Zhong
Evidence-Based Complementary and Alternative Medicine.2015; 2015: 1. CrossRef - Type 2 Diabetes Mellitus, Metabolic Syndrome, and Mixed Dyslipidemia: How Similar, How Different, and How to Treat?
Julian Halcox, Anoop Misra
Metabolic Syndrome and Related Disorders.2015; 13(1): 1. CrossRef - How to balance cardiorenometabolic benefits and risks of statins
Soo Lim, Pyung Chun Oh, Ichiro Sakuma, Kwang Kon Koh
Atherosclerosis.2014; 235(2): 644. CrossRef - Contemporary treatment strategies for Type 2 diabetes-related macrovascular disease
Andrew MN Walker, Richard M Cubbon, Mark T Kearney
Expert Review of Endocrinology & Metabolism.2014; 9(6): 641. CrossRef
- High doses of rosuvastatin induce impaired branched‐chain amino acid catabolism and lead to insulin resistance
- Predicting Mortality of Critically Ill Patients by Blood Glucose Levels
- Byung Sam Park, Ji Sung Yoon, Jun Sung Moon, Kyu Chang Won, Hyoung Woo Lee
- Diabetes Metab J. 2013;37(5):385-390. Published online October 17, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.5.385
- 3,454 View
- 34 Download
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The aim of this study is to observe the outcome of critically ill patients in relation to blood glucose level at admission and to determine the optimal range of blood glucose at admission predicting lower hospital mortality among critically ill patients.
Methods We conducted a retrospective cohort study of a total 1,224 subjects (males, 798; females, 426) admitted to intensive care unit (ICU) from 1 January 2009 to 31 December 2010. Blood glucose levels at admission were categorized into four groups (group 1, <100 mg/dL; group 2, 100 to 199 mg/dL; group 3, 200 to 299 mg/dL; and group 4, ≥300 mg/dL).
Results Among 1,224 patients, 319 patients were already known diabetics, and 296 patients died in ICU. Five hundred fifty-seven subjects received insulin therapy, and 118 received oral hypoglycemic agents. The overall mortality rate was 24.2% (296 patients). The causes of death and mortality rates of diabetic patients were not different from nondiabetic subjects. The mortality curve showed J shape, and there were significant differences in mortality between the groups of blood glucose levels at admission. Group 2 had the lowest mortality rate (
P <0.05).Conclusion These results suggest that serum glucose levels upon admission into ICU is associated with clinical outcomes in ICU patients. Blood glucose level between 100 and 199 mg/dL at the time of ICU admission could predict lower hospital mortality among critically ill patients.
-
Citations
Citations to this article as recorded by- HGV4Risk: Hierarchical Global View-guided Sequence Representation Learning for Risk Prediction
Youru Li, Zhenfeng Zhu, Xiaobo Guo, Shaoshuai Li, Yuchen Yang, Yao Zhao
ACM Transactions on Knowledge Discovery from Data.2024; 18(1): 1. CrossRef - Feature extraction from unequal length heterogeneous EHR time series via dynamic time warping and tensor decomposition
Chi Zhang, Hadi Fanaee-T, Magne Thoresen
Data Mining and Knowledge Discovery.2021; 35(4): 1760. CrossRef - Serum electrolytes levels in patients with type 2 diabetes mellitus: a cross-sectional study
Shridhar Reshma, Sushith Sushith, Mangalore Balakrishna Prathima, D'Sa Janice, Gopal R Madan, Pragathi Gowda, Kiran PK Kumar, Mohandas Rai, Bhuvanesh Sukhlal Kalal
Diabetes mellitus.2020; 23(3): 223. CrossRef - Systemic Corticosteroids and Mortality in Severe and Critical COVID-19 Patients in Wuhan, China
Jianfeng Wu, Jianqiang Huang, Guochao Zhu, Yihao Liu, Han Xiao, Qian Zhou, Xiang Si, Hui Yi, Cuiping Wang, Daya Yang, Shuling Chen, Xin Liu, Zelong Liu, Qiongya Wang, Qingquan Lv, Ying Huang, Yang Yu, Xiangdong Guan, Yanbing Li, Krishnarajah Nirantharakum
The Journal of Clinical Endocrinology & Metabolism.2020; 105(12): e4230. CrossRef - Derivation and validation of a new nutritional index for predicting 90 days mortality after ICU admission in a Korean population
Da-Hye Son, Kyung-Sub Kim, Hye-Sun Lee, Ji-Won Lee, Cheung-Soo Shin
Journal of the Formosan Medical Association.2020; 119(8): 1283. CrossRef - Acute pancreatic beta cell apoptosis by IL-1β is responsible for postburn hyperglycemia: Evidence from humans and mice
Jun Li, Jie Xu, Xinghua Qin, Hongyan Yang, Juntao Han, Yanhui Jia, Huayu Zhu, Liang Zhu, Jia Li, Wenjun Xie, Dahai Hu, Xing Zhang, Feng Gao
Biochimica et Biophysica Acta (BBA) - Molecular Basis of Disease.2019; 1865(2): 275. CrossRef - Determinants of mortality in patients with type 2 diabetes: a review
Jana Engelmann, Ulf Manuwald, Constanze Rubach, Joachim Kugler, Andreas L. Birkenfeld, Markolf Hanefeld, Ulrike Rothe
Reviews in Endocrine and Metabolic Disorders.2016; 17(1): 129. CrossRef - The Impact of Measurement Frequency on the Domains of Glycemic Control in the Critically Ill-A Monte Carlo Simulation
James S. Krinsley, David E. Bruns, James C. Boyd
Journal of Diabetes Science and Technology.2015; 9(2): 237. CrossRef - Response: Predicting Mortality of Critically Ill Patients by Blood Glucose Levels (Diabetes Metab J2013;37:385-90)
Byung Sam Park, Ji Sung Yoon
Diabetes & Metabolism Journal.2014; 38(1): 81. CrossRef - Predicting Mortality of Critically Ill Patients by Blood Glucose Levels (Diabetes Metab J2013;37:385-90)
Hyeong Kyu Park
Diabetes & Metabolism Journal.2013; 37(6): 484. CrossRef
- HGV4Risk: Hierarchical Global View-guided Sequence Representation Learning for Risk Prediction
- The Role of Skeletal Muscle in Development of Nonalcoholic Fatty Liver Disease
- Jun Sung Moon, Ji Sung Yoon, Kyu Chang Won, Hyoung Woo Lee
- Diabetes Metab J. 2013;37(4):278-285. Published online August 14, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.4.278
- 4,637 View
- 49 Download
- 58 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Nonalcoholic fatty liver disease (NAFLD) is closely correlated with abnormal accumulation of visceral fat, but the role of skeletal muscle remains unclear. The aim of this study was to elucidate the role of skeletal muscle in development of NAFLD.
Methods Among 11,116 subjects (6,242 males), we examined the effects of skeletal muscle mass and visceral fat area (VFA, by bioelectric impedance analysis) on NAFLD using by the fatty liver index (FLI).
Results Of the total subjects (9,565 total, 5,293 males) included, 1,848 were classified as having NALFD (FLI ≥60). Body mass index, lipid profile, fasting plasma glucose, hemoglobin A1c, prevalence of type 2 diabetes (DM), hypertension (HTN), and metabolic syndrome were higher in males than females, but FLI showed no significant difference. The low FLI group showed the lowest VFA and highest skeletal muscle mass of all the groups. Skeletal muscle to visceral fat ratio (SVR) and skeletal muscle index had inverse correlations with FLI, when adjusted for age and gender. In multivariate regression analysis, SVR was negatively associated with FLI. Among SVR quartiles, the highest quartile showed very low risk of NAFLD when adjusted for age, gender, lipid profile, DM, HTN, and high sensitivity C-reactive protein from the lowest quartiles (odds ratio, 0.037; 95% confidence interval, 0.029 to 0.049).
Conclusion Skeletal muscle mass was inversely associated with visceral fat area, and higher skeletal muscle mass may have a beneficial effect in preventing NAFLD. These results suggest that further studies are needed to ameliorate or slow the progression of sarcopenia.
-
Citations
Citations to this article as recorded by- Effects of nonalcoholic fatty liver disease on sarcopenia: evidence from genetic methods
Jiaqin Yuan, Jinglin Zhang, Qiang Luo, Lipeng Peng
Scientific Reports.2024;[Epub] CrossRef - Influence of Sugar-Sweetened Beverages Intake on Sarcopenic Obesity, Visceral Obesity, and Sarcopenia in Lebanese Patients with MASLD: A Case-Control Study
Maha Hoteit, Myriam Dagher, Nikolaos Tzenios, Najat Al Kaaki, Ghadir Rkein, Abdul Rahman Chahine, Yonna Sacre, Samer Hotayt, Rami Matar, Mahmoud Hallal, Micheal Maitar, Bilal Hotayt
Healthcare.2024; 12(5): 591. CrossRef - Increased visceral fat area to skeletal muscle mass ratio is positively associated with the risk of metabolic dysfunction-associated steatotic liver disease in a Chinese population
Chenbing Liu, Nan Li, Di Sheng, Yahong Shao, Lihong Qiu, Chao Shen, Zhong Liu
Lipids in Health and Disease.2024;[Epub] CrossRef - Using hyperhomocysteinemia and body composition to predict the risk of non-alcoholic fatty liver disease in healthcare workers
Xiaoyan Hao, Honghai He, Liyuan Tao, Peng Wang
Frontiers in Endocrinology.2023;[Epub] CrossRef - Diagnostic Criteria and Prognostic Relevance of Sarcopenia in Patients with Inflammatory Bowel Disease—A Systematic Review
Claudia-Gabriela Potcovaru, Petruța Violeta Filip, Oana-Maria Neagu, Laura Sorina Diaconu, Teodor Salmen, Delia Cinteză, Anca Pantea Stoian, Florin Bobirca, Mihai Berteanu, Corina Pop
Journal of Clinical Medicine.2023; 12(14): 4713. CrossRef - Association between Muscle Mass Deficits and Metabolic Dysfunction-Associated Fatty Liver Disease in Adults with Body Mass Index Less than 23 kg/m2
Mi Young Lee, Hee Jeong Choi, Han Jin Oh
Korean Journal of Family Practice.2023; 13(3): 171. CrossRef - Sex influences the association between appendicular skeletal muscle mass to visceral fat area ratio and non-alcoholic steatohepatitis in patients with biopsy-proven non-alcoholic fatty liver disease
Gang Li, Rafael S. Rios, Xin-Xin Wang, Yue Yu, Kenneth I. Zheng, Ou-Yang Huang, Liang-Jie Tang, Hong-Lei Ma, Yi Jin, Giovanni Targher, Christopher D. Byrne, Xiao-Yan Pan, Ming-Hua Zheng
British Journal of Nutrition.2022; 127(11): 1613. CrossRef - 2019 Global NAFLD Prevalence: A Systematic Review and Meta-analysis
Michael H. Le, Yee Hui Yeo, Xiaohe Li, Jie Li, Biyao Zou, Yuankai Wu, Qing Ye, Daniel Q. Huang, Changqing Zhao, Jie Zhang, Chenxi Liu, Na Chang, Feng Xing, Shiping Yan, Zi Hui Wan, Natasha Sook Yee Tang, Maeda Mayumi, Xinting Liu, Chuanli Liu, Fajuan Rui,
Clinical Gastroenterology and Hepatology.2022; 20(12): 2809. CrossRef - Impact of Sarcopenia and Myosteatosis in Non-Cirrhotic Stages of Liver Diseases: Similarities and Differences across Aetiologies and Possible Therapeutic Strategies
Annalisa Cespiati, Marica Meroni, Rosa Lombardi, Giovanna Oberti, Paola Dongiovanni, Anna Ludovica Fracanzani
Biomedicines.2022; 10(1): 182. CrossRef - Impact of Sarcopenia on the Severity of the Liver Damage in Patients With Non-alcoholic Fatty Liver Disease
Vittoria Zambon Azevedo, Cristina Alina Silaghi, Thomas Maurel, Horatiu Silaghi, Vlad Ratziu, Raluca Pais
Frontiers in Nutrition.2022;[Epub] CrossRef - Fatty Liver Index and Skeletal Muscle Density
Julie A. Pasco, Sophia X. Sui, Emma C. West, Kara B. Anderson, Pamela Rufus-Membere, Monica C. Tembo, Natalie K. Hyde, Lana J. Williams, Zoe S. J. Liu, Mark A. Kotowicz
Calcified Tissue International.2022; 110(6): 649. CrossRef - Skeletal muscle mass to visceral fat area ratio as a predictor of NAFLD in lean and overweight men and women with effect modification by sex
Yoosun Cho, Yoosoo Chang, Seungho Ryu, Hyun‐Suk Jung, Chan‐won Kim, Hyungseok Oh, Mi Kyung Kim, Won Sohn, Hocheol Shin, Sarah H. Wild, Christopher D. Byrne
Hepatology Communications.2022; 6(9): 2238. CrossRef - Association of Low Skeletal Muscle Mass with the Phenotype of Lean Non-Alcoholic Fatty Liver Disease
Jun-Hyeon Byeon, Min-Kyu Kang, Min-Cheol Kim
Healthcare.2022; 10(5): 850. CrossRef - Muscle strength, but not body mass index, is associated with mortality in patients with non‐alcoholic fatty liver disease
Phunchai Charatcharoenwitthaya, Khemajira Karaketklang, Wichai Aekplakorn
Journal of Cachexia, Sarcopenia and Muscle.2022; 13(5): 2393. CrossRef - Effect of progressive resistance training with weight loss compared with weight loss alone on the fatty liver index in older adults with type 2 diabetes: secondary analysis of a 12-month randomized controlled trial
Christine L Freer, Elena S George, Sze-Yen Tan, Gavin Abbott, David W Dunstan, Robin M Daly
BMJ Open Diabetes Research & Care.2022; 10(5): e002950. CrossRef - Muscle Krüppel-like factor 15 regulates lipid flux and systemic metabolic homeostasis
Liyan Fan, David R. Sweet, Domenick A. Prosdocimo, Vinesh Vinayachandran, Ernest R. Chan, Rongli Zhang, Olga Ilkayeva, Yuan Lu, Komal S. Keerthy, Chloe E. Booth, Christopher B. Newgard, Mukesh K. Jain
Journal of Clinical Investigation.2021;[Epub] CrossRef - “Bioelectrical impedance analysis in managing sarcopenic obesity in NAFLD”
David J. Hanna, Scott T. Jamieson, Christine S. Lee, Christopher A. Pluskota, Nicole J. Bressler, Peter N. Benotti, Sandeep Khurana, David D. K. Rolston, Christopher D. Still
Obesity Science & Practice.2021; 7(5): 629. CrossRef - Decreased Muscle-to-Fat Mass Ratio Is Associated with Low Muscular Fitness and High Alanine Aminotransferase in Children and Adolescent Boys in Organized Sports Clubs
Kai Ushio, Yukio Mikami, Hiromune Obayashi, Hironori Fujishita, Kouki Fukuhara, Tetsuhiko Sakamitsu, Kazuhiko Hirata, Yasunari Ikuta, Hiroaki Kimura, Nobuo Adachi
Journal of Clinical Medicine.2021; 10(11): 2272. CrossRef - Association of Skeletal Muscle and Adipose Tissue Distribution with Histologic Severity of Non-Alcoholic Fatty Liver
Min-Kyu Kang, Jung-Hun Baek, Young-Oh Kweon, Won-Young Tak, Se-Young Jang, Yu-Rim Lee, Keun Hur, Gyeonghwa Kim, Hye-Won Lee, Man-Hoon Han, Joon-Hyuk Choi, Soo-Young Park, Jung-Gil Park
Diagnostics.2021; 11(6): 1061. CrossRef - Association of Body Composition and Sarcopenia with NASH in Obese Patients
Sophia Marie-Therese Schmitz, Lena Schooren, Andreas Kroh, Alexander Koch, Christine Stier, Ulf Peter Neumann, Tom Florian Ulmer, Patrick Hamid Alizai
Journal of Clinical Medicine.2021; 10(15): 3445. CrossRef - Patchouli alcohol ameliorates skeletal muscle insulin resistance and NAFLD via AMPK/SIRT1-mediated suppression of inflammation
Do Hyeon Pyun, Tae Jin Kim, Seung Yeon Park, Hyun Jung Lee, A.M. Abd El-Aty, Ji Hoon Jeong, Tae Woo Jung
Molecular and Cellular Endocrinology.2021; 538: 111464. CrossRef - Hepatic Steatosis Contributes to the Development of Muscle Atrophy via Inter-Organ Crosstalk
Kenneth Pasmans, Michiel E. Adriaens, Peter Olinga, Ramon Langen, Sander S. Rensen, Frank G. Schaap, Steven W. M. Olde Damink, Florian Caiment, Luc J. C. van Loon, Ellen E. Blaak, Ruth C. R. Meex
Frontiers in Endocrinology.2021;[Epub] CrossRef - Muscle mass and cellular membrane integrity assessment in patients with nonalcoholic fatty liver disease
Iasmin dos Santos Barreto, Raquel Oliveira dos Santos, Raquel Rocha, Claudineia de Souza, Naiade Almeida, Luiza Valois Vieira, Rafael Leiróz, Manoel Sarno, Carla Daltro, Helma Pinchemel Cotrim
Revista da Associação Médica Brasileira.2021; 67(9): 1233. CrossRef - A significant association of non-obese non-alcoholic fatty liver disease with sarcopenic obesity
Kazuhiro Kashiwagi, Michiyo Takayama, Kayoko Fukuhara, Ryoko Shimizu-Hirota, Po-Sung Chu, Nobuhiro Nakamoto, Nagamu Inoue, Yasushi Iwao, Takanori Kanai
Clinical Nutrition ESPEN.2020; 38: 86. CrossRef - Improvement in Menopause-Associated Hepatic Lipid Metabolic Disorders by Herbal Formula HPC03 on Ovariectomized Rats
BoYoon Chang, Dae Sung Kim, SungYeon Kim
Evidence-Based Complementary and Alternative Medicine.2020; 2020: 1. CrossRef - Sarcopenia is associated with non-alcoholic fatty liver disease in men with type 2 diabetes
D.H. Seo, Y.-h. Lee, S.W. Park, Y.J. Choi, B.W. Huh, E. Lee, K.B. Huh, S.H. Kim, B.-S. Cha
Diabetes & Metabolism.2020; 46(5): 362. CrossRef - Nonalcoholic fatty liver disease and sarcopenia: pathophysiological connections and therapeutic implications
Tiziana Fernández-Mincone, Felipe Contreras-Briceño, Maximiliano Espinosa-Ramírez, Patricio García-Valdés, Antonio López-Fuenzalida, Arnoldo Riquelme, Juan Pablo Arab, Daniel Cabrera, Marco Arrese, Francisco Barrera
Expert Review of Gastroenterology & Hepatology.2020; 14(12): 1141. CrossRef - Association between Atrial Fibrillation and Advanced Liver Fibrosis in Patients with Non-Alcoholic Fatty Liver Disease
Min Kyu Kang, Jung Gil Park, Min Cheol Kim
Yonsei Medical Journal.2020; 61(10): 860. CrossRef - Relative fat mass at baseline and its early change may be a predictor of incident nonalcoholic fatty liver disease
Hwi Young Kim, Su Jung Baik, Hye Ah Lee, Byoung Kwon Lee, Hye Sun Lee, Tae Hun Kim, Kwon Yoo
Scientific Reports.2020;[Epub] CrossRef - Fisetin Alleviates Hepatic and Adipocyte Fibrosis and Insulin Resistance in Diet-Induced Obese Mice
Myung-Sook Choi, Ji-Young Choi, Eun-Young Kwon
Journal of Medicinal Food.2020; 23(10): 1019. CrossRef - Relationship between relative skeletal muscle mass and nonalcoholic fatty liver disease: a systematic review and meta-analysis
Changzhou Cai, Xin Song, Yishu Chen, Xueyang Chen, Chaohui Yu
Hepatology International.2020; 14(1): 115. CrossRef - Sarcopenia Is a New Risk Factor of Nonalcoholic Fatty Liver Disease in Patients with Inflammatory Bowel Disease
Min Kyu Kang, Kyeong Ok Kim, Min Cheol Kim, Jung Gil Park, Byung Ik Jang
Digestive Diseases.2020; 38(6): 507. CrossRef - Relationship between Muscle Mass/Strength and Hepatic Fat Content in Post-Menopausal Women
Yajie Zhang, Dajiang Lu, Renwei Wang, Weijie Fu, Shengnian Zhang
Medicina.2019; 55(10): 629. CrossRef - Lower hand grip strength in older adults with non-alcoholic fatty liver disease: a nationwide population-based study
Beom-Jun Kim, Seong Hee Ahn, Seung Hun Lee, Seongbin Hong, Mark W. Hamrick, Carlos M. Isales, Jung-Min Koh
Aging.2019; 11(13): 4547. CrossRef - Nonalcoholic Fatty Liver Disease in Nonobese Subjects of African Origin Has Atypical Metabolic Characteristics
Debbie S Thompson, Ingrid A Tennant, Deanne P Soares, Clive Osmond, Chris D Byrne, Terrence E Forrester, Michael S Boyne
Journal of the Endocrine Society.2019; 3(11): 2051. CrossRef - Sarcopenia in patients with non‐alcoholic fatty liver disease: is it a clinically significant entity?
C. H. De Fré, M. A. De Fré, W. J. Kwanten, B. J. Op de Beeck, L. F. Van Gaal, S. M. Francque
Obesity Reviews.2019; 20(2): 353. CrossRef - Nonalcoholic Fatty Liver Disease in The Rotterdam Study: About Muscle Mass, Sarcopenia, Fat Mass, and Fat Distribution
Louise Johanna Maria Alferink, Katerina Trajanoska, Nicole Stephanie Erler, Josje Dorothea Schoufour, Robert Jacobus de Knegt, M. Arfan Ikram, Harry Leonardus Antonius Janssen, Oscar H. Franco, Herold J. Metselaar, Fernando Rivadeneira, Sarwa Darwish Mura
Journal of Bone and Mineral Research.2019; 34(7): 1254. CrossRef - Sarcopenia Is Significantly Associated with Presence and Severity of Nonalcoholic Fatty Liver Disease
Goh Eun Chung, Min Joo Kim, Jeong Yoon Yim, Joo Sung Kim, Ji Won Yoon
Journal of Obesity & Metabolic Syndrome.2019; 28(2): 129. CrossRef - Association of low skeletal muscle mass with advanced liver fibrosis in patients with non‐alcoholic fatty liver disease
Min Kyu Kang, Jung Gil Park, Heon Ju Lee, Min Cheol Kim
Journal of Gastroenterology and Hepatology.2019; 34(9): 1633. CrossRef - Whole‐body vibration for patients with nonalcoholic fatty liver disease: a 6‐month prospective study
Sechang Oh, Natsumi Oshida, Noriko Someya, Tsuyoshi Maruyama, Tomonori Isobe, Yoshikazu Okamoto, Taeho Kim, Bokun Kim, Junichi Shoda
Physiological Reports.2019; 7(9): e14062. CrossRef - L-Lysine Attenuates Hepatic Steatosis in Senescence-Accelerated Mouse Prone 8 Mice
Tomonori SATO, Nao MURAMATSU, Yoshiaki ITO, Yoshio YAMAMOTO, Takashi NAGASAWA
Journal of Nutritional Science and Vitaminology.2018; 64(3): 192. CrossRef - Short-term treatment with metformin reduces hepatic lipid accumulation but induces liver inflammation in obese mice
Alexandre Abilio de Souza Teixeira, Camila O. Souza, Luana A. Biondo, Loreana Sanches Silveira, Edson A. Lima, Helena A. Batatinha, Adriane Pereira Araujo, Michele Joana Alves, Sandro Massao Hirabara, Rui Curi, José Cesar Rosa Neto
Inflammopharmacology.2018; 26(4): 1103. CrossRef - Vitamin D and Related Deficiencies, Sarcopenia and Visceral Obesity in Obese People with NAFLD
Mihaela Petrova
Gastroenterology & Hepatology: Open Access.2018;[Epub] CrossRef - Grip Strength Moderates the Association between Anthropometric and Body Composition Indicators and Liver Fat in Youth with an Excess of Adiposity
Robinson Ramírez-Vélez, Mikel Izquierdo, Jorge Correa-Bautista, Alejandra Tordecilla-Sanders, María Correa-Rodríguez, Jacqueline Schmidt Rio-Valle, Emilio González-Jiménez, Katherine González-Ruíz
Journal of Clinical Medicine.2018; 7(10): 347. CrossRef - Longitudinal Changes in Muscle Mass and Strength, and Bone Mass in Older Adults: Gender-Specific Associations Between Muscle and Bone Losses
Kyoung Min Kim, Soo Lim, Tae Jung Oh, Jae Hoon Moon, Sung Hee Choi, Jae Young Lim, Ki Woong Kim, Kyong Soo Park, Hak Chul Jang
The Journals of Gerontology: Series A.2018; 73(8): 1062. CrossRef - Non-alcoholic fatty liver disease connections with fat-free tissues: A focus on bone and skeletal muscle
Eleonora Poggiogalle, Lorenzo Maria Donini, Andrea Lenzi, Claudio Chiesa, Lucia Pacifico
World Journal of Gastroenterology.2017; 23(10): 1747. CrossRef - Sarcopenia and non-alcoholic fatty liver disease: Is there a relationship? A systematic review
Cristiane V Tovo, Sabrina A Fernandes, Caroline Buss, Angelo A de Mattos
World Journal of Hepatology.2017; 9(6): 326. CrossRef - Multiple molecular targets in the liver, adipose tissue and skeletal muscle in ginger-elicited amelioration of nonalcoholic fatty liver disease
Chunxia Wang, Robert Batey, Johji Yamahara, Yuhao Li
Journal of Functional Foods.2017; 36: 43. CrossRef - Importance of Lean Muscle Maintenance to Improve Insulin Resistance by Body Weight Reduction in Female Patients with Obesity
Yaeko Fukushima, Satoshi Kurose, Hiromi Shinno, Ha Cao Thu, Nana Takao, Hiromi Tsutsumi, Yutaka Kimura
Diabetes & Metabolism Journal.2016; 40(2): 147. CrossRef - Fatty Liver Index Associates with Relative Sarcopenia and GH/ IGF- 1 Status in Obese Subjects
Eleonora Poggiogalle, Carla Lubrano, Lucio Gnessi, Stefania Mariani, Andrea Lenzi, Lorenzo Maria Donini, Rasheed Ahmad
PLOS ONE.2016; 11(1): e0145811. CrossRef - The relationship between hepatic steatosis and skeletal muscle mass index in men with type 2 diabetes
Yoshitaka Hashimoto, Takafumi Osaka, Takuya Fukuda, Muhei Tanaka, Masahiro Yamazaki, Michiaki Fukui
Endocrine Journal.2016; 63(10): 877. CrossRef - Sarcopenia and the cardiometabolic syndrome: A narrative review
G. Bahat, B. İlhan
European Geriatric Medicine.2016; 7(3): 220. CrossRef - Low skeletal muscle mass is associated with non-alcoholic fatty liver disease in Korean adults: the Fifth Korea National Health and Nutrition Examination Survey
Hee Yeon Kim, Chang Wook Kim, Chung-Hwa Park, Jong Young Choi, Kyungdo Han, Anwar T Merchant, Yong-Moon Park
Hepatobiliary & Pancreatic Diseases International.2016; 15(1): 39. CrossRef - Non-alcoholic fatty liver disease and cardiovascular risk: Pathophysiological mechanisms and implications
Sven M. Francque, Denise van der Graaff, Wilhelmus J. Kwanten
Journal of Hepatology.2016; 65(2): 425. CrossRef - Differences among skeletal muscle mass indices derived from height-, weight-, and body mass index-adjusted models in assessing sarcopenia
Kyoung Min Kim, Hak Chul Jang, Soo Lim
The Korean Journal of Internal Medicine.2016; 31(4): 643. CrossRef - Relationship between grip strength and newly diagnosed nonalcoholic fatty liver disease in a large-scale adult population
Ge Meng, Hongmei Wu, Liyun Fang, Chunlei Li, Fei Yu, Qing Zhang, Li Liu, Huanmin Du, Hongbin Shi, Yang Xia, Xiaoyan Guo, Xing Liu, Xue Bao, Qian Su, Yeqing Gu, Huijun Yang, Bin Yu, Yuntang Wu, Zhong Sun, Kaijun Niu
Scientific Reports.2016;[Epub] CrossRef - Volume-dependent effect of supervised exercise training on fatty liver and visceral adiposity index in subjects with type 2 diabetes The Italian Diabetes Exercise Study (IDES)
Stefano Balducci, Patrizia Cardelli, Luca Pugliese, Valeria D’Errico, Jonida Haxhi, Elena Alessi, Carla Iacobini, Stefano Menini, Lucilla Bollanti, Francesco G. Conti, Antonio Nicolucci, Giuseppe Pugliese
Diabetes Research and Clinical Practice.2015; 109(2): 355. CrossRef - Sarcopenia is a risk factor for elevated aminotransferase in men independently of body mass index, dietary habits, and physical activity
Ki Deok Yoo, Dae Won Jun, Kang Nyeong Lee, Hang Lak Lee, Oh Young Lee, Byung Chul Yoon, Ho Soon Choi
Digestive and Liver Disease.2015; 47(4): 303. CrossRef
- Effects of nonalcoholic fatty liver disease on sarcopenia: evidence from genetic methods
- The Relationship between Metformin and Cancer in Patients with Type 2 Diabetes
- Hyun Hee Chung, Jun Sung Moon, Ji Sung Yoon, Hyoung Woo Lee, Kyu Chang Won
- Diabetes Metab J. 2013;37(2):125-131. Published online April 16, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.2.125
- 3,557 View
- 29 Download
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Recently, several studies reported that the cancer incidence in type 2 diabetes patients is higher than in the general population. Although a number of risks are shared between cancer and diabetes patients, there have been few studies of its correlation. We evaluated the influences of several factors including low density lipoprotein cholesterol (LDL-C), albuminuria and use of metformin on the risk of cancer in patients with type 2 diabetes.
Methods We enrolled 1,320 patients with at least 5 years of follow-up and 73 patients were diagnosed with cancer during this period. The associations of the risk factors with cancer incidence were evaluated by multiple regression analysis. The subjects were placed into two subgroups based on metformin dosage (<1,000 mg/day, ≥1,000 mg/day) and we compared cancer incidence using analysis of covariance.
Results LDL-C and albuminuria were not significantly correlated with cancer risk. In contrast, metformin showed a reverse correlation with cancer risk (
P =0.006; relative risk, 0.574). In the metformin nonadministration group, smoking, male gender, and high triglyceride levels tended to be contributing factors without statistical significance. Cancer occurence was lower in the low dose metformin group (less than 1,000 mg/day) (P =0.00).Conclusion These results suggest that the administration of low dose metformin in patients with type 2 diabetes may be associated with a reduced risk of cancer.
-
Citations
Citations to this article as recorded by- Metformin Reduces Tumor Growth in a Murine Flank Schwannoma Model
Sudhir Manickavel, Yolanda Hartman, Andrew Burns, Manuel A. Lora Gonzalez, Jason Warram, Erika Walsh, Jacob B. Hunter, Daniel E. Killeen
Otology & Neurotology.2023; 44(9): 941. CrossRef - Metformin induces TPC-1 cell apoptosis through endoplasmic reticulum stress-associated pathways in vitro and in vivo
Jianwen Ye, Lei Qi, Kunlun Chen, Renfeng Li, Shengping Song, Chuang Zhou, Wenlong Zhai
International Journal of Oncology.2019;[Epub] CrossRef - Metformin Promotes Apoptosis but Suppresses Autophagy in Glucose-Deprived H4IIE Hepatocellular Carcinoma Cells
Deok-Bae Park
Diabetes & Metabolism Journal.2015; 39(6): 518. CrossRef - Combination Therapy of Metformin and Statin May Decrease Hepatocellular Carcinoma Among Diabetic Patients in Asia
Hsin-Hung Chen, Ming-Chia Lin, Chih-Hsin Muo, Su-Yin Yeh, Fung-Chang Sung, Chia-Hung Kao
Medicine.2015; 94(24): e1013. CrossRef - mitoNEET as a novel drug target for mitochondrial dysfunction
Werner J. Geldenhuys, Thomas C. Leeper, Richard T. Carroll
Drug Discovery Today.2014; 19(10): 1601. CrossRef - Diabetes - Increased Risk for Cancers through Chromosomal Aberrations?
Sudhaa Anand, Badari Nath, Radha Saraswathy
Asian Pacific Journal of Cancer Prevention.2014; 15(11): 4571. CrossRef - Oleanolic Acid Induces Metabolic Adaptation in Cancer Cells by Activating the AMP-Activated Protein Kinase Pathway
Jia Liu, Lanhong Zheng, Ning Wu, Leina Ma, Jiateng Zhong, Ge Liu, Xiukun Lin
Journal of Agricultural and Food Chemistry.2014; 62(24): 5528. CrossRef - Association of Vitamin B12Deficiency and Metformin Use in Patients with Type 2 Diabetes
Sun-Hye Ko, Sun-Hee Ko, Yu-Bae Ahn, Ki-Ho Song, Kyung-Do Han, Yong-Moon Park, Seung-Hyun Ko, Hye-Soo Kim
Journal of Korean Medical Science.2014; 29(7): 965. CrossRef - Metformin and Cancer Risk and Mortality: A Systematic Review and Meta-analysis Taking into Account Biases and Confounders
Sara Gandini, Matteo Puntoni, Brandy M. Heckman-Stoddard, Barbara K. Dunn, Leslie Ford, Andrea DeCensi, Eva Szabo
Cancer Prevention Research.2014; 7(9): 867. CrossRef - Effects of Metformin on CD133+ Colorectal Cancer Cells in Diabetic Patients
Yanfei Zhang, Meiping Guan, Zongji Zheng, Qian Zhang, Fang Gao, Yaoming Xue, Chunming Liu
PLoS ONE.2013; 8(11): e81264. CrossRef - AACE Comprehensive Diabetes Management Algorithm 2013 Endocrine Practice
Héctor Eloy Tamez-Pérez, Stephanie Lissette Proskauer-Peña, Mayra Ivonne Hernández-Coria
Endocrine Practice.2013; 19(4): 736. CrossRef - Complications of Diabetes Therapy
Sarah D. Corathers, Shawn Peavie, Marzieh Salehi
Endocrinology and Metabolism Clinics of North America.2013; 42(4): 947. CrossRef - Metformin and Cancer in Type 2 Diabetes
Hyeong Kyu Park
Diabetes & Metabolism Journal.2013; 37(2): 113. CrossRef
- Metformin Reduces Tumor Growth in a Murine Flank Schwannoma Model
- Diagnostic Accuracy of 64-Slice MDCT Coronary Angiography for the Assessment of Coronary Artery Disease in Korean Patients with Type 2 Diabetes
- Jun Sung Moon, Ji Sung Yoon, Kyu Chang Won, Ihn-Ho Cho, Hyoung Woo Lee
- Diabetes Metab J. 2013;37(1):54-62. Published online February 15, 2013
- DOI: https://doi.org/10.4093/dmj.2013.37.1.54
- 3,663 View
- 29 Download
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background A 64-slice multidetector computed tomography (MDCT) is well known to be a useful noninvasive form of angiography for the general population, but not for certain patients with diabetes. The aim of this study was to investigate the diagnostic accuracy and usefulness of 64-slice MDCT coronary angiography for detecting coronary artery disease in Korean patients with type 2 diabetes mellitus (T2DM).
Methods A total of 240 patients were included, 74 of whom had type 2 diabetes (M:F=40:33; 41.8±9.5 years). We compared significant coronary stenosis (>50% luminal narrowing) in MDCT with invasive coronary angiography (ICA) by segment, artery, and patient. We also evaluated the influence of obesity and coronary calcium score on MDCT accuracy.
Results Of the 4,064 coronary segments studied, 4,062 segments (T2DM=1,109) were assessed quantitatively by both MDCT and ICA, and 706 segments (T2DM=226) were detected as a significant lesion by ICA in all patients. Sensitivity, specificity, as well as positive and negative predictive values for the presence of significant stenosis in T2DM were: by segment, 89.4%, 96.4%, 85.8%, and 97.4%, respectively; by artery (
n =222), 95.1%, 92.9%, 94.4%, and 93.8%, respectively; by patients (n =74), 98.4%, 100.0%, 98.4%, and 90.0%, respectively. Regardless of presence of diabetes, there was no significant difference in diagnostic accuracy. Obesity (≥25 kg/m2) and coronary calcium score did not also affect the diagnostic accuracy of MDCT.Conclusion The 64-slice MDCT coronary angiography was found to have similar diagnostic accuracy with ICA, regardless of diabetes. These results suggest MDCT may be helpful to reduce unnecessary invasive studies for patients with diabetes.
-
Citations
Citations to this article as recorded by- Can Radiation Dose Burden of CT Angiography be Reduced While Still Accurately Diagnosing Etiology of Acute Chest Pain?
Sherine M. Sharara, Scott R. Monnin, Manolo Rubio, Rami N. Khouzam, Samar R. Ragheb
Current Problems in Cardiology.2021; 46(4): 100766. CrossRef - Assessment of high sensitivity C-reactive protein and coronary plaque characteristics by computed tomography in patients with and without diabetes mellitus
Hai-Ting Zhou, De-Li Zhao, Guo-Kun Wang, Tian-Zuo Wang, Hong-Wei Liang, Jin-Ling Zhang
BMC Cardiovascular Disorders.2020;[Epub] CrossRef - Triglyceride Glucose-Waist Circumference Better Predicts Coronary Calcium Progression Compared with Other Indices of Insulin Resistance: A Longitudinal Observational Study
Yun Kyung Cho, Jiwoo Lee, Hwi Seung Kim, Eun Hee Kim, Min Jung Lee, Dong Hyun Yang, Joon-Won Kang, Chang Hee Jung, Joong-Yeol Park, Hong-Kyu Kim, Woo Je Lee
Journal of Clinical Medicine.2020; 10(1): 92. CrossRef - The impact of non-alcoholic fatty liver disease and metabolic syndrome on the progression of coronary artery calcification
Yun Kyung Cho, Yu Mi Kang, Jee Hee Yoo, Jiwoo Lee, Seung Eun Lee, Dong Hyun Yang, Joon-Won Kang, Joong-Yeol Park, Chang Hee Jung, Hong-Kyu Kim, Woo Je Lee
Scientific Reports.2018;[Epub] CrossRef - Effects of Low-density Lipoprotein Cholesterol on Coronary Artery Calcification Progression According to High-density Lipoprotein Cholesterol Levels
Da Young Lee, Ji Hyun Kim, Se Eun Park, Cheol-young Park, Ki-won Oh, Sung-woo Park, Eun-Jung Rhee, Won-young Lee
Archives of Medical Research.2017; 48(3): 284. CrossRef - 2013 ACC/AHA Cholesterol Guideline Versus 2004 NCEP ATP III Guideline in the Prediction of Coronary Artery Calcification Progression in a Korean Population
Yun Kyung Cho, Chang Hee Jung, Yu Mi Kang, Jenie Yoonoo Hwang, Eun Hee Kim, Dong Hyun Yang, Joon‐Won Kang, Joong‐Yeol Park, Hong‐Kyu Kim, Woo Je Lee
Journal of the American Heart Association.2016;[Epub] CrossRef - Imaging Quality Evaluation of Low Tube Voltage Coronary CT Angiography Using Low Concentration Contrast Medium
Chengzhong Zhang, Yuejun Yu, Zaixian Zhang, Qingguo Wang, Linfeng Zheng, Yan Feng, Zhiguo Zhou, Guixiang Zhang, Kangan Li, Zhuoli Zhang
PLOS ONE.2015; 10(3): e0120539. CrossRef - 2013 ACC/AHA versus 2004 NECP ATP III Guidelines in the Assignment of Statin Treatment in a Korean Population with Subclinical Coronary Atherosclerosis
Chang Hee Jung, Min Jung Lee, Yu Mi Kang, Dong Hyun Yang, Joon-Won Kang, Eun Hee Kim, Duk-Woo Park, Joong-Yeol Park, Hong-Kyu Kim, Woo Je Lee, Yingmei Feng
PLOS ONE.2015; 10(9): e0137478. CrossRef - Serum Total Bilirubin Levels Provide Additive Risk Information over the Framingham Risk Score for Identifying Asymptomatic Diabetic Patients at Higher Risk for Coronary Artery Stenosis
Jaechan Leem, Eun Hee Koh, Jung Eun Jang, Chang-Yun Woo, Jin Sun Oh, Min Jung Lee, Joon-Won Kang, Tae-Hwan Lim, Chang Hee Jung, Woo Je Lee, Joong-Yeol Park, Ki-Up Lee
Diabetes & Metabolism Journal.2015; 39(5): 414. CrossRef - Association between serum gamma-glutamyltransferase and the progression of coronary artery calcification
Yun Kyung Cho, Yu Mi Kang, Jenie Yoonoo Hwang, Eun Hee Kim, Dong Hyun Yang, Joon-Won Kang, Joong-Yeol Park, Woo Je Lee, Hong-Kyu Kim, Chang Hee Jung
Atherosclerosis.2015; 243(1): 300. CrossRef - Role of Bilirubin in Diabetic Vascular Complications: Can Bilirubin Predict More than Just Liver Disease?
Jun Sung Moon
Diabetes & Metabolism Journal.2015; 39(5): 384. CrossRef - The Association of Rate of Weight Gain During Early Adulthood With the Prevalence of Subclinical Coronary Artery Disease in Recently Diagnosed Type 2 Diabetes: The MAXWEL-CAD Study
Soo Lim, Sung Hee Choi, Kyoung Min Kim, Sang Il Choi, Eun Ju Chun, Min Joo Kim, Kyong Soo Park, Hak Chul Jang, Naveed Sattar
Diabetes Care.2014; 37(9): 2491. CrossRef - Retraction: Diagnostic Accuracy of 64-Slice MDCT Coronary Angiography for the Assessment of Coronary Artery Disease in Korean Patients with Type 2 Diabetes
Jun Sung Moon, Ji Sung Yoon, Kyu Chang Won, Ihn-Ho Cho, Hyoung Woo Lee
Diabetes & Metabolism Journal.2013; 37(3): 217. CrossRef
- Can Radiation Dose Burden of CT Angiography be Reduced While Still Accurately Diagnosing Etiology of Acute Chest Pain?
- Understanding the Cardiovascular Effects of Incretin
- Ji Sung Yoon, Hyoung Woo Lee
- Diabetes Metab J. 2011;35(5):437-443. Published online October 31, 2011
- DOI: https://doi.org/10.4093/dmj.2011.35.5.437
- 3,272 View
- 43 Download
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Cardiovascular disease (CVD), a leading cause of death in patients with diabetes mellitus, has several pathogenic mechanisms that are well established. However, the traditional hypoglycemic agents do not have proven positive effects on macrovascular disease. Novel therapeutic agents target the incretin pathway including the glucagon-like peptide 1 (GLP-1) receptor (GLP-1R) agonists and the dipeptidyl peptidase-4 inhibitors. The glucose-regulatory actions of these agents function by increasing insulin secretion and suppressing glucagon. They also act to increase weight loss not only by inhibiting gastric emptying, but also by reducing appetite. Although GLP-1 and GLP-1R agonists have demonstrated beneficial effects on myocardium and vascular endothelium including coronary and peripheral mouse vessels, they also have anti-inflammatory and anti-atherogenic actions. These agents also have positive effects on the lipid profile and blood pressure. Although these cardioprotective actions seem to be beyond the effects of glucose control and weight loss, they are mediated through GLP-1R- or GLP-1R-independent actions of cleaved GLP-1 (9-36). Larger randomized controlled trials are necessary to elucidate the clinical promise of these beneficial CVD effects.
-
Citations
Citations to this article as recorded by- Cardioprotective Effects of Glucagon-like Peptide-1 (9-36) Against Oxidative Injury in H9c2 Cardiomyoblasts: Potential Role of the PI3K/Akt/NOS Pathway
Narawat Nuamnaichati, Warisara Parichatikanond, Supachoke Mangmool
Journal of Cardiovascular Pharmacology.2022; 79(1): e50. CrossRef - Comparisons of pleiotropic effects of SGLT2 inhibition and GLP-1 agonism on cardiac glucose intolerance in heart dysfunction
Belma Turan, Aysegul Durak, Yusuf Olgar, Erkan Tuncay
Molecular and Cellular Biochemistry.2022; 477(11): 2609. CrossRef - Interrelations of components of metabolic syndrome with the level of the hormones involved in regulation of adipose tissue metabolism
A. Y. Babenko, G. A. Matveev, T. I. Alekseenko, I. V. Derevitskii, M. A. Kokina, E. V. Shlyakhto
"Arterial’naya Gipertenziya" ("Arterial Hypertension").2020; 25(6): 639. CrossRef - Attenuation of carotid neointimal formation after direct delivery of a recombinant adenovirus expressing glucagon-like peptide-1 in diabetic rats
Soo Lim, Gha Young Lee, Ho Seon Park, Dong-Hwa Lee, Oh Tae Jung, Kim Kyoung Min, Young-Bum Kim, Hee-Sook Jun, Jang Hak Chul, Kyong Soo Park
Cardiovascular Research.2017; 113(2): 183. CrossRef - Renoprotective Effects of the Dipeptidyl Peptidase-4 Inhibitor Sitagliptin: A Review in Type 2 Diabetes
Cristina Mega, Edite Teixeira-de-Lemos, Rosa Fernandes, Flávio Reis
Journal of Diabetes Research.2017; 2017: 1. CrossRef - Letter: Economic Impact of Combining Metformin with Dipeptidyl Peptidase-4 Inhibitors in Diabetic Patients with Renal Impairment in Spanish Patients (Diabetes Metab J2015;39:74-81)
Hannah Seok
Diabetes & Metabolism Journal.2015; 39(2): 171. CrossRef - Diuretic and Natriuretic Effects of Dipeptidyl Peptidase-4 Inhibitor Teneligliptin
Masao Moroi, Tetsuya Kubota
Journal of Cardiovascular Pharmacology.2015; 66(2): 159. CrossRef - The Nonglycemic Actions of Dipeptidyl Peptidase-4 Inhibitors
Na-Hyung Kim, Taeyang Yu, Dae Ho Lee
BioMed Research International.2014; 2014: 1. CrossRef - Tolerability, effectiveness and predictive parameters for the therapeutic usefulness of exenatide in obese, Korean patients with type 2 diabetes
Sun Ok Song, Kwang Joon Kim, Byung‐Wan Lee, Eun Seok Kang, Bong Soo Cha, Hyun Chul Lee
Journal of Diabetes Investigation.2014; 5(5): 554. CrossRef - The endothelium in diabetes: Its role in insulin access and diabetic complications
Cathryn M. Kolka, Richard N. Bergman
Reviews in Endocrine and Metabolic Disorders.2013; 14(1): 13. CrossRef - Is GPR119 agonism an appropriate treatment modality for the safe amelioration of metabolic diseases?
Lauren M Cornall, Michael L Mathai, Deanne H Hryciw, Andrew J McAinch
Expert Opinion on Investigational Drugs.2013; 22(4): 487. CrossRef - Effects of GLP-1 on Forearm Vasodilator Function and Glucose Disposal During Hyperinsulinemia in the Metabolic Syndrome
Manfredi Tesauro, Francesca Schinzari, Angelo Adamo, Valentina Rovella, Francesca Martini, Nadia Mores, Angela Barini, Dario Pitocco, Giovanni Ghirlanda, Davide Lauro, Umberto Campia, Carmine Cardillo
Diabetes Care.2013; 36(3): 683. CrossRef - Effect of a Dipeptidyl Peptidase-IV Inhibitor, Des-Fluoro-Sitagliptin, on Neointimal Formation after Balloon Injury in Rats
Soo Lim, Sung Hee Choi, Hayley Shin, Bong Jun Cho, Ho Seon Park, Byung Yong Ahn, Seon Mee Kang, Ji Won Yoon, Hak Chul Jang, Young-Bum Kim, Kyong Soo Park, Alice Y. W. Chang
PLoS ONE.2012; 7(4): e35007. CrossRef - Glucagon-like peptide 1 and cardiac cell survival
Susana Ravassa, Amaia Zudaire, Javier Díez
Endocrinología y Nutrición (English Edition).2012; 59(9): 561. CrossRef - GLP-1 and cardioprotection: from bench to bedside
S. Ravassa, A. Zudaire, J. Diez
Cardiovascular Research.2012; 94(2): 316. CrossRef - Saxagliptin improves glucose tolerance but not survival in a murine model of dilated cardiomyopathy
Arpita Kalla Vyas, Lauren B. Aerni-Flessner, Maria A. Payne, Attila Kovacs, Patrick Y. Jay, Paul W. Hruz
Cardiovascular Endocrinology.2012; 1(4): 74. CrossRef - Péptido similar al glucagón tipo 1 y supervivencia de la célula cardiaca
Susana Ravassa, Amaia Zudaire, Javier Díez
Endocrinología y Nutrición.2012; 59(9): 561. CrossRef
- Cardioprotective Effects of Glucagon-like Peptide-1 (9-36) Against Oxidative Injury in H9c2 Cardiomyoblasts: Potential Role of the PI3K/Akt/NOS Pathway
- The Combination of Fasting Plasma Glucose and Glycosylated Hemoglobin as a Predictor for Type 2 Diabetes in Korean Adults.
- Chan Hee Lee, Woo Jin Chang, Hyun Hee Chung, Hyun Jung Kim, Sang Hyun Park, Jun Sung Moon, Ji Eun Lee, Ji Sung Yoon, Kyung Ah Chun, Kyu Chang Won, Ihn Ho Cho, Hyoung Woo Lee
- Korean Diabetes J. 2009;33(4):306-314. Published online August 1, 2009
- DOI: https://doi.org/10.4093/kdj.2009.33.4.306
- 3,120 View
- 24 Download
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The oral glucose tolerance test (OGTT) for detection of diabetes is difficult to perform in clinical settings. The aim of this study is to evaluate the performance of a more practical detection test, combined fasting plasma glucose (FPG) and glycosylated hemoglobin (HbA1c), as a predictor of diabetes mellitus (DM) in a Korean sample. METHODS: We examined 2,045 (M = 1,276, mean age = 47.8 +/- 9.0 yrs) medical check-up program participants between January 2002 to December 2003. FPG, HbA1c and a number of other biochemical tests were performed at baseline and four after years after initial screening. Patients who originally presented with diabetes were excluded. The characteristics of newly-diagnosed DM patients and non-diabetic patients were compared. RESULTS: The incidence of newly diagnosed diabetes was 1.6% (32/2,045) after four years of follow up. The subjects in the DM group were older, had higher levels of SBP, DBP, FPG, HbA1c, triglyceride, HDL cholesterol, GGT and LDH (P < 0.05). In multivariate logistic regression analysis, FPG (odds ratio [OR] 1.124) and HbA1c (OR 4.794) were significantly correlated with onset of diabetes (P < 0.05). The interaction parameter between FPG and HbA1c was more than 1.0, indicating that the two effects are synergistic. The predictive cut-off values of HbA1c and FPG were 5.35% (area under curve [AUC] = 0.944) and 102.5 mg/dL (AUC = 0.930), respectively. CONCLUSION: The combination of HbA1c above 5.35% and FPG above 102.5 mg/dL predicted the onset of diabetes in a Korean sample. These results suggest that the combination of FPG and HbA1c may be useful for predicting progression to type 2 diabetes in east Asians. -
Citations
Citations to this article as recorded by- The Distribution and Characteristics of Abnormal Findings Regarding Fasting Plasma Glucose and HbA1c - Based on Adults Except for Known Diabetes
Seyoung Kwon, Youngak Na
The Korean Journal of Clinical Laboratory Science.2017; 49(3): 239. CrossRef - Factors Affecting Diabetic Screening Behavior of Korean Adults: A Multilevel Analysis
Hyeongsu Kim, Minjung Lee, Haejoon Kim, Kunsei Lee, Sounghoon Chang, Vitna Kim, Jun Pyo Myong, Soyoun Jeon
Asian Nursing Research.2013; 7(2): 67. CrossRef - Impact of HbA1c Criterion on the Detection of Subjects with Increased Risk for Diabetes among Health Check-Up Recipients in Korea
Hong-Kyu Kim, Sung-Jin Bae, Jaeone Choe
Diabetes & Metabolism Journal.2012; 36(2): 151. CrossRef - The Utility of HbA1c as a Diagnostic Criterion of Diabetes
Hee-Jung Kim, Eun Young Choi, Eal Whan Park, Yoo Seock Cheong, Hong-Yoen Lee, Ji Hyun Kim
Korean Journal of Family Medicine.2011; 32(7): 383. CrossRef - Predictive Clinical Parameters for the Therapeutic Efficacy of Sitagliptin in Korean Type 2 Diabetes Mellitus
Soon Ae Kim, Woo Ho Shim, Eun Hae Lee, Young Mi Lee, Sun Hee Beom, Eun Sook Kim, Jeong Seon Yoo, Ji Sun Nam, Min Ho Cho, Jong Suk Park, Chul Woo Ahn, Kyung Rae Kim
Diabetes & Metabolism Journal.2011; 35(2): 159. CrossRef - Optimal range of HbA1c for the prediction of future diabetes: A 4-year longitudinal study
Ji Cheol Bae, Eun Jung Rhee, Won Young Lee, Se Eun Park, Cheol Young Park, Ki Won Oh, Sung Woo Park, Sun Woo Kim
Diabetes Research and Clinical Practice.2011; 93(2): 255. CrossRef - The Combination of Fasting Plasma Glucose and Glycosylated Hemoglobin as a Predictor for Type 2 Diabetes in Korean Adults (Korean Diabetes J 33(4):306-314, 2009)
Soo Lim
Korean Diabetes Journal.2009; 33(5): 448. CrossRef - The Combination of Fasting Plasma Glucose and Glycosylated Hemoglobin as a Predictor for Type 2 Diabetes in Korean Adults (Korean Diabetes J 33(4):306-314, 2009)
Chan Hee Lee, Hyoung Woo Lee
Korean Diabetes Journal.2009; 33(5): 451. CrossRef
- The Distribution and Characteristics of Abnormal Findings Regarding Fasting Plasma Glucose and HbA1c - Based on Adults Except for Known Diabetes
- Relationship Between Serum Bilirubin Levels and Coronary Atherosclerosis in Patients with Type 2 Diabetes.
- Jun Sung Moon, Woo Jin Chang, Chan Hee Lee, Ji Eun Lee, Kyung Ah Chun, Ji Sung Yoon, Ihn Ho Cho, Hyoung Woo Lee, Kyu Chang Won
- Korean Diabetes J. 2008;32(4):338-345. Published online August 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.4.338
- 2,519 View
- 18 Download
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Lipid oxidation and formation of oxygen radicals have been identified to be the important factors of atherogenesis. Because bilirubin, a potent physiological antioxidant inhibits lipid oxidation, it is suggested that low serum concentrations of bilirubin is associated with atherosclerosis. The aim of this study was to evaluate the relationship between bilirubin levels and coronary atherosclerosis. METHODS: The coronary calcium score (CCS) of 172 subjects (male 63, mean age 60.5 +/- 1.0) with type 2 diabetes were evaluated in Yeungnam University Hospital between January 2005 and February 2007. The subjects were divided into two groups with CCS 10 as the cut off. RESULTS: Higher CCS was significantly associated with lower bilirubin (P < 0.05), but after adjusted with age, no longer correlation were seen (P = 0.121). To determine the relationship between subclinical coronary atherosclerosis and bilirubin, the subjects with previous history of cardiovascular disease were excluded. In 138 subjects (male 54, mean age 58.4 +/- 1.1), higher CCS was significantly associated with lower levels of bilirubin. After adjusted with age, duration of diabetes, and history of hypertension, CCS was also inversely related with bilirubin (P < 0.05). CONCLUSION: These results suggest that lower levels of bilirubin might be considered as a risk factor of coronary artery disease, especially in type 2 diabetics without cardiovascular disease. -
Citations
Citations to this article as recorded by- Effects of Ginseng By-Products Supplementation on Performance,
Blood Biochemical Profiles, Organ Development, and Stress Parameter in
Broiler under Heat Stress Condition
Jun-Ho Lee, Ji-Won Yoon, Bong-Ki Kim, Hee-Bok Park, Kyu-Sang Lim, Ji-Hyuk Kim
Korean Journal of Poultry Science.2022; 49(4): 255. CrossRef - Correlation of Serum Bilirubin Levels in Type 2 Diabetes Mellitus Patients with and without Diabetic Retinopathy
Johncy John, Gajaraj Tulsidas Naik, Suria C. Rashmi, Sheetal Vaijanath Zille, Swetha Sampangi Iyer, Meghana Neeralagi, Asma M.K
Journal of Evolution of Medical and Dental Sciences.2021; 10(45): 4013. CrossRef - Association of SNPs in the UGT1A gene cluster with total bilirubin and mortality in the Diabetes Heart Study
Amanda J. Cox, Maggie C.-Y. Ng, Jianzhao Xu, Carl D. Langefeld, Kenneth L. Koch, Paul A. Dawson, J. Jeffrey Carr, Barry I. Freedman, Fang-Chi Hsu, Donald W. Bowden
Atherosclerosis.2013; 229(1): 155. CrossRef - The Association between Low Serum Bilirubin and Carotid Atherosclerosis in Subjects with Type 2 Diabetes
Byoung Hyun Park, Hye Jung Nho, Chung Gu Cho
Endocrinology and Metabolism.2012; 27(2): 126. CrossRef - Association of Serum Total Bilirubin with Serum High Sensitivity C-reactive Protein in Middle-aged Men
Kiwoong Yu, Cheolhwan Kim, Eunju Sung, Hocheol Shin, Hyewon Lee
Korean Journal of Family Medicine.2011; 32(6): 327. CrossRef - The Relationship among Homocysteine, Bilirubin, and Diabetic Retinopathy
Ho Chan Cho
Diabetes & Metabolism Journal.2011; 35(6): 595. CrossRef - Relationship Between Serum Bilirubin Levels and Coronary Atherosclerosis in Patients with Type 2 Diabetes (Korean Diabetes Journal 32(4):338-345, 2008)
Soo Lim
Korean Diabetes Journal.2008; 32(5): 462. CrossRef
- Effects of Ginseng By-Products Supplementation on Performance,
Blood Biochemical Profiles, Organ Development, and Stress Parameter in
Broiler under Heat Stress Condition
- Clinical Significance of Decreased Glomerular Filtration Rate (GFR) without Albuminuria among Type 2 Diabetics.
- Ji Eun Lee, Kyu Chang Won, Hyoung Woo Lee, Ji Sung Yoon
- Korean Diabetes J. 2008;32(3):252-258. Published online June 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.3.252
- 2,328 View
- 22 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Microalbuminuria in type 2 diabetes is a predictor of development of clinical nephropathy and cardiovascular disease. But, it has been reported that reduced glomerular filtration rate (GFR) may occur in some normoalbuminuric diabetic patients. The aim of this study was to identify whether decreased GFR without microalbuminuria is to predict diabetic vascular complications. METHODS: Between January 1998 and February 2001, 73 patients with type 2 diabetes who visited Yeungnam university medical center were divided into 5 groups according to initial GFR ranges: group 1 (GFR < 30 mL/min), group 2 (30 < or = GFR < 60 mL/min), group 3 (60 < or = GFR < 90 mL/min), group 4 (90 < or = GFR < 125 mL/min), group 5 (125 mL/min < or = GFR). They were examined for microvascular and macrovascular complications initially and after 4 years. RESULTS: Decreased GFR had a negative correlation with age (r = -0.472, P = 0.001). Decreased GFR without microalbuminuria had a significant correlation with development of diabetic nephropathy (P = 0.016) after 4 years. There were no significant correlation with the prevalence of diabetic retinopathy, peripheral neuropathy, and macrovacular disease. But, our study showed that coronary artery disease had an increasing tendency with decreased GFR without statistical significance (P = 0.085). CONCLUSIONS: Our data suggest that reduced GFR, independent of albuminuria, may be an important predictor of diabetic nephropathy and coronary artery disease to some extent. So we recommend that not only the microalbuminuria, but also the decrease in GFR should be evaluated at the follow-up of patients with type 2 diabetes. -
Citations
Citations to this article as recorded by- Screening and Management of Diabetic Nephropathy
Ji Sung Yoon
The Journal of Korean Diabetes.2013; 14(1): 19. CrossRef
- Screening and Management of Diabetic Nephropathy
- Glucose Toxicity and Pancreatic Beta Cell Dysfunction in Type 2 Diabetes.
- Kyu Chang Won, Ji Sung Yoon
- Korean Diabetes J. 2008;32(3):175-181. Published online June 1, 2008
- DOI: https://doi.org/10.4093/kdj.2008.32.3.175
- 2,360 View
- 38 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - The adverse effects of prolonged exposure of pancreatic islets to supraphysiologic glucose concentrations (i.e. glucose toxicity) is mediated at least in part by glucose oxidation and the subsequent generation of reactive oxygen species (ROS) that can impair insulin gene expression and beta cell function. Multiple biochemical pathways and mechanisms of action for glucose toxicity have been suggested. These include glucose autoxidation, protein kinase C activation, methylglyoxal formation and glycation, hexosamine metabolism, sorbitol formation, and oxidative phosphorylation. There are many potential mechanisms whereby excess glucose metabolites traveling along these pathways might cause beta cell damage. However, all these pathways have in common the formation of reactive oxygen species that, in excess and over time, cause chronic oxidative stress, which in turn causes defective insulin gene expression and insulin secretion as well as increased apoptosis. The intracellular peroxide levels of the pancreatic islets (INS-1 cells, rat islets) by flow cytometry were increased in the high glucose media compared to 5.6 mM glucose media. The insulin, MafA, PDX-1 mRNA levels and glucose stimulated insulin secretion (GSIS) were decreased in high glucose media compared to 5.6 mM glucose media. The HO-1 seems to mediate the protective response of pancreatic islets against the oxidative stress that is due to high glucose conditions. Also, we observed decreased glutathione level, gamma-GCS expression and increased oxidized LDL, malondialdehyde level at leukocytes and mesothelial cells from patients with Korean Type 2 Diabetes (esp, poorly controlled patients). In conclusion, this pathophysiologic sequence sets the scene for considering antioxidant therapy as an adjunct in the management of diabetes, especially type 2 Diabetes.
-
Citations
Citations to this article as recorded by- Factors That Influence Pancreatic Beta Cell Function and Insulin Resistance in Newly Diagnosed Type 2 Diabetes Patients: A Sub-Analysis of the MARCH Trial
Yan Duan, Jia Liu, Yuan Xu, Ning Yang, Wenying Yang, Guang Wang
Diabetes Therapy.2018; 9(2): 743. CrossRef - Effects of 8 Weeks Resistance Exercise on GSH, SOD, TBARS Activities and GLUT2 mRNA Expression of Pancreas in OLETF Rats
Min-Ki Lee, Jin-Hwan Yoon
The Korean Journal of Physical Education.2017; 56(3): 551. CrossRef - Determining the Factors that Influence the Insulin Requirements in Type 2 Diabetic Patients
Jin Ook Chung, Dong Hyeok Cho, Dong Jin Chung, Min Young Chung
Endocrinology and Metabolism.2010; 25(2): 110. CrossRef - The Effects of Weight Training by Intensity for 8 Weeks of Metabolic Syndrome Factor Improvement in Overweight High School Students
Journal of Life Science.2009; 19(4): 492. CrossRef
- Factors That Influence Pancreatic Beta Cell Function and Insulin Resistance in Newly Diagnosed Type 2 Diabetes Patients: A Sub-Analysis of the MARCH Trial

 KDA
KDA
 First
First Prev
Prev





